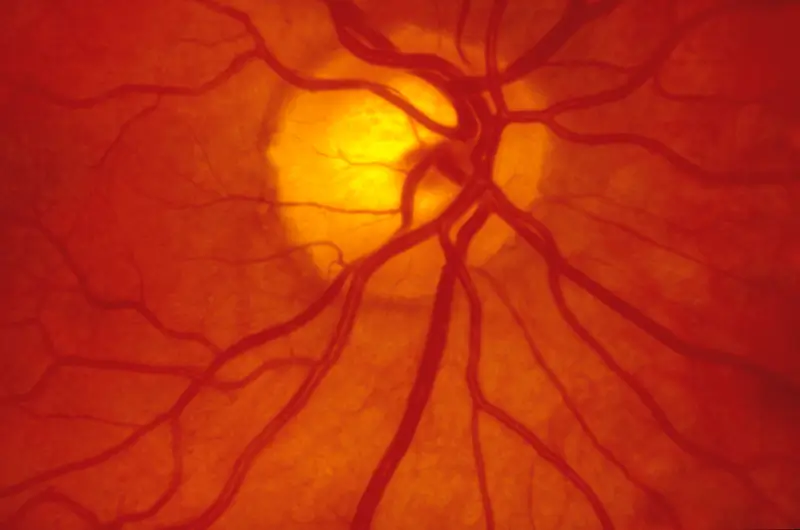
Diabetic retinopathy is an eye condition that can affect people with Type 1 or Type 2 diabetes. It occurs when uncontrolled high blood sugar levels damage the blood vessels that nourish the retina. The blood vessels can swell and leak or close, cutting off blood supply to the retina. New blood vessels can grow, but not develop properly. The condition, if not managed properly, can lead to loss of vision. To get appropriately reimbursed, ophthalmologists should make sure that the patient’s medical record contains sufficient documentation to support the need for treatment. Ophthalmology medical billing and coding outsourcing can ensure timely and accurate claim submission for optimal reimbursement for the medical services provided.
Symptoms and Stages
Risk of developing diabetic retinopathy can increase due to duration of diabetes, poorly controlled blood sugar level, high blood pressure and cholesterol levels, pregnancy, tobacco use, and other factors.
Symptoms may be absent in the early stages, but will develop as the condition progresses. The common symptoms of diabetic retinopathy include:
- Spots or dark strings floating in vision (floaters)
- Blurred vision
- Fluctuating vision
- Impaired color vision
- Dark or empty areas in vision
- Vision loss
The two main stages of diabetic eye disease are: NPDR (non-proliferative diabetic retinopathy) and PDR (proliferative diabetic retinopathy).
- NPDR (non-proliferative diabetic retinopathy) is early stage of diabetic eye disease. It is non-proliferative as new blood vessels are not growing. The walls of the retina weaken and tiny bulges extend outwards, sometimes leaking blood and fluid into the retina. Larger retinal vessels can extend abnormally. The severity of NPDR can increase as more blood vessels get blocked. Fluid build-up in the central part of the retina (macular edema) will cause swelling and blur vision and requires treatment.
- PDR (proliferative diabetic retinopathy) is the advanced stage of diabetic eye disease. This stage is characterized by neovascularization – the growth of new blood vessels on the surface of the retina. These delicate new vessels bleed very easily and usually progress into loss of vision. These new blood vessels can also cause scar tissue to form. Scar tissue can lead to retinal detachment. PDR is a very serious complication, and can block both central and peripheral (side) vision.
Diagnosis and Treatment
- Diagnosis: Ophthalmologists conduct a comprehensive dilated eye exam to diagnose diabetic retinopathy. Drops will be put in the eye to dilate the pupil, and the inside of the eye will be examined through a lens to check for:
- Abnormal blood vessels
- Swelling, blood or fatty deposits in the retina
- Growth of new blood vessels and scar tissue
- Bleeding in the clear, jelly-like substance that fills the center of the eye (vitreous)
- Retinal detachment
- Abnormalities in the optic nerve
- Cataracts
- Glaucoma
Fluorescein angiography may be used to check for leaks, blocks, and abnormal growth of blood vessels. Another test, optical coherence tomography (OCT) provides detailed images of the thickness of the retina and allows the physician to measure swelling. Vision tests may also be conducted.
- Treatment: Treatment for diabetic retinopathy depends on the severity of the condition.
- Mild or moderate nonproliferative diabetic retinopathy: If the condition is not serious, it can be usually managed with blood sugar control. Controlling blood sugar with medication and diet can slow progression.
- Advanced diabetic retinopathy: Treatment for advanced diabetic retinopathy includes photocoagulation, panretinal photocoagulation, vitrectomy, and Anti-VEGF therapy.
- Photocoagulation or focal laser treatment involves using laser burns to stop/slow the leakage of blood and fluid in the eye and prevent macular edema from getting worse.
- Panretinal photocoagulation or scatter laser treatment treats the areas of the retina away from the macula in order to shrink the abnormal new blood vessels. The treatment may cause some loss of peripheral vision or night vision.
- Vitrectomy is an eye operation conducted to remove blood inside the eye and replacing it with a saline solution. This will allow the light to reach the retina and improve vision. The procedure is done in a surgical center or hospital under local or general anesthesia.
- Injecting medications: Injecting vascular endothelial growth factor (VEGF) inhibitors into the eyemay help stop growth of new blood vessels, reduce macular swelling and possibly improve vision.
Diabetic Retinopathy – ICD-10 and CPT codes
The documentation should clearly show if diabetic retinopathy is proliferative or nonproliferative, if nonproliferative, is it mild, moderate, or severe, and whether there macular edema. For appropriate reimbursement, providers should ensure that the diagnostic, procedure, and therapeutic codes on insurance billing claims for diabetic retinopathy accurately reflect services provided.
Diabetic Retinopathy ICD-10 Codes
The ICD-10 codes for diabetic retinopathy are listed in the diabetes section (E08-E13) of Chapter 4, Endocrine, Nutritional and Metabolic Diseases, while the most common retinal complications are in Chapter 7. There are ICD-10 codes for nonproliferative diabetic retinopathy (NPDR), proliferative diabetic retinopathy (PDR), wet age-related macular degeneration (AMD), and dry age-related macular degeneration (AMD). There are many codes under the following code sets for diabetic retinopathy:
Retinopathy E11.319 – Type 2 diabetes mellitus with unspecified diabetic retinopathy without macular edema
-
- Nonproliferative E11.329
- mild E11.329
- with macular edema E11.321
- moderate E11.339
- with macular edema E11.331
- severe E11.349
- with macular edema E11.341
- with macular edema E11.321
- mild E11.329
- Proliferative E11.359
With:- combined traction retinal detachment and rhegmatogenous retinal detachment E11.354
- macular edema E11.351
- stable proliferative diabetic retinopathy E11.355
- traction retinal detachment involving the macula E11.352
- traction retinal detachment not involving the macula E11.353
- with macular edema E11.311, and
- with macular edema resolved following treatment E11.37
- Vitreous hemorrhage H43.1
The billable ICD-10 codes for vitreous hemorrhage are:- H43.10 Vitreous hemorrhage, unspecified eye
- H43.11 Vitreous hemorrhage, right eye
- H43.12 Vitreous hemorrhage, left eye
- H43.13 Vitreous hemorrhage, bilateral
- Nonproliferative E11.329
Specifying Laterality
Under ICD-10, laterality is an important component in code selection. It’s crucial to select the appropriate eye (right or left) for getting appropriate reimbursement. For example:
-
-
- E10.3211: Type 1 diabetes mellitus with mild nonproliferative diabetic retinopathy with macular edema right eye
- E10.3292: Type 1 diabetes mellitus with mild nonproliferative diabetic retinopathy without macular edema, left eye
-
Diabetic Retinopathy CPT Codes
Posterior segment laser photocoagulation is performed to treat focal or panretinal diabetic retinopathy and surrounding retinal holes or tears to prevent retinal detachments. Laser photocoagulation is also used to treat macular edema. The key CPT codes for laser photocoagulation are:
-
-
- 67105 Repair of retinal detachment, including drainage of subretinal fluid when performed; photocoagulation
- 67145 Prophylaxis of retinal detachment (eg, retinal break, lattice degeneration) w/o drainage, 1 or more sessions; photocoagulation
- 67210 Destruction of localized lesion of retina (eg, macular edema, tumors), 1 or more sessions; photocoagulation
- 67220 Destruction of localized lesion of choroid (eg, choroidal neovascularization); photocoagulation 1 or more sessions
- 67228 Treatment of extensive or progressive retinopathy; (eg diabetic retinopathy), photocoagulation
- 67229 Treatment of extensive or progressive retinopathy, 1 or more sessions, preterm infant; (less than 37 weeks gestation at birth), performed from birth up to 1 year of age (eg, retinopathy of prematurity), photocoagulation or cryotherapy
-
Other diabetic retinopathy laser procedure codes:
Outpatient Surgery Magazine recently listed other relevant laser treatment codes:
-
-
- 66821 YAG capsulotomy surgery: using a YAG laser to ablate the tissue in the posterior capsule to reopen the visual pathway. The procedure is generally performed not less than 90 days following cataract extraction. YAG performed less than 90 days following cataract extraction should meet both the indications and limitations of this LCD.
- 65855 Selective laser trabeculoplasty – performed on glaucoma patients to open up the trabecular meshwork in order to increase fluid outflow.
- 66761 Laser peripheral iridotomy – performed on glaucoma patients to create a hole in the iris to lower intracular pressure by letting fluid flow out from the back of the eye.
- 67210 Focal photocoagulation – a 520nm laser is used to destroy damaged eye tissue and remove scarring that contributes to blind spots and vision loss
-
Vitrectomy procedure codes include:
-
-
- 66852 Removal of lens material; pars plana approach, with or without vitrectomy
- 67036 Vitrectomy, mechanical, pars plana approach
- 67039 Vitrectomy, mechanical, pars plana approach; with focal endolaser photocoagulation
- 67040 Vitrectomy, mechanical, pars plana approach; with endolaserpanretinal
photocoagulation - 67041 Vitrectomy, mechanical, pars plana approach; with removal of preretinal cellular
-
Medicare and other payers cover laser photocoagulation and other procedures for the proper indications and when supported by the medical record. However, with multiple codes and documentation requirements, billing and coding for diabetic retinopathy can be extremely challenging. Many providers find it difficult to understand the modifiers, indicators, and terminology used in determining Medicare payment for ophthalmic diagnostic tests. Ophthalmologists also need to check private payer or Medicare Advantage (MA) coverage guidance before initiating treatment and determine if prior authorization is required. Outsourcing medical billing and coding to an experienced service provider is a feasible strategy to manage these challenges and ensure optimal reimbursement.