2,500,000+
Verifications
500+
Practices
Years
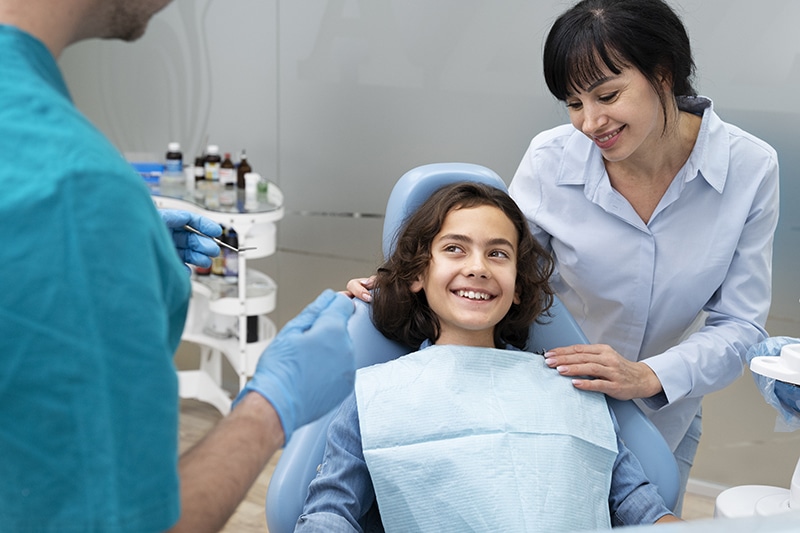
Simplify Your Dental Insurance and Eligibility Verifications
We eliminate the need for you to negotiate the complex payer systems or endure long hold times. By leveraging our one-click verification platform and backup phone verification support, we help your practice stay 3–5 days ahead of patient schedules.
Our Comprehensive Dental Eligibility Verification Services
- Coverage start and end dates
- Waiting periods and frequency limitations
- Annual maximums and remaining benefits
- Copayments and coinsurance
- Deductibles and met status
- Exclusions and pre-authorization requirements
OSI – EXPERIENCED DENTAL INSURANCE VERIFICATION PARTNER
Who We Are
With our services, you have:
- A resolute team and project manager
- Customized turnaround times
- No long-term agreements or contracts
- Competitive pricing
- Ongoing QA and reports
Why Choose Us?
Direct EMR Integration
Dedicated communication channel
Human + AI Support
Dental Software We Support













Ortho & Oral






How Do You Price Your Verification Services
As a dental insurance verification company since 2001, we understand that every practice is different and one pricing may not work for all. With our transparent pricing and customizable packages, we will optimize your dental verification services pricing to fit your needs.
Fixed Cost Pricing
Our Proven Dental Insurance Verification Process
1
Review Patient
Schedules
Check
Priority
Check Eligibility
& Verify
Update
Coverage Tables
Quality Control
Reporting
Review Patient Schedules
Check Priority
Check Eligibility and Verify (Online & Calls)
Update Coverage Tables
Quality Control Reporting
We serve all 50 states
FAQs
What dental software are you familiar with?
We have experience working on various software:
Dental
Dentrix
Dentrix Enterprise
Dentrix Ascend
Eaglesoft
Open Dental
Curve Dental
SoftDent
Denticon
Easy Dental
Carestream Dental
Dentisoft Office Cloud
DentiMax
Digital Office
Ortho & Oral
OMSVision- Maxillo
OrthoTrac
OrthoEdge
DSN
Cloud 9
Dolphin
Can you use our verification forms?
How do we know that you are experienced in our specialty?
When it comes to Dentistry, we have experience in all specialties and nuances of their procedures. We are presently providing services to Family dentists, Pediatric dentists, Orthodontists, Oral surgeons, Periodontists, Endodontists, Prosthodontists and so on.
Don’t take our word for it. Ask us about our free trial and make sure you are comfortable with our capabilities.
What does your support look like?
Do you have any restrictions on dental insurance coverage information you capture?
How can I get started?
Are you HIPAA compliant?
What are your contract terms?
Why is it important to verify a patient's dental insurance?
By conducting dental insurance verification, the dental practice can review a patient’s benefits information prior to treatment, reducing the risk of last-minute cancellations, co-pay rejections, claim denials, and delays.
Do you provide coverage in all US states?
What is the process of insurance verification?
When did OSI come into existence?
What does the startup process with your company look like?
How extensive can your insurance verification be?
Where are you located?
Can OSI educate patients on insurance coverage?
Related Posts
Importance of Insurance Verification in Dental Practices
by Amber Darst | Posted: Nov 05, 2024
Five Compelling Reasons to Outsource Dental Insurance Verification
by Amber Darst | Posted: Jul 25, 2024