Healthcare providers and patients often report difficulties with health insurers regarding prior authorizations, with many consumers saying their care was either denied or delayed last year, due to the requirements in pre-authorizations. Keeping the existing concerns and problems in mind, the federal government body, Centers for Medicare & Medicaid Services (CMS) released the CMS Interoperability and Prior Authorization Final Rule (CMS-0057-F) earlier this year. This new regulation aims to improve electronic exchange of health information and streamlines the prior authorization process for medical items and services. The new requirements of this regulation are obligatory for Medicare Advantage (MA) organizations, state Medicaid fee for-service (FFS) programs, state Children’s Health Insurance Program (CHIP) FFS programs, Medicaid managed care plans, CHIP managed care entities, and Qualified Health Plan (QHP) issuers on the Federally facilitated Exchanges (FFEs).
It is estimated that the new policies issued by this government agency will improve patient access to health information and prior authorization processes to reduce the burden on patients, healthcare providers and insurers along with saving approximately $15 billion for physician practices over the next ten years. This rule, however, comes with a set of limitations as the final rule does not address prior authorization requirements for the following:
- prescription drugs
- health plan variation for services that require pre-authorization
- lack of clarity on the usage of technologies for automated process
- potential security and privacy risks of patient information due to electronic data exchange
- appeals of prior authorization denials
The PA process for approval of high-cost specialty medications is burdensome, and costs pharmacies and physicians’ practices a lot in terms of time and money. Pharmacy prior authorization distracts from patient care, can delay care and even cause patients to abandon treatment. Outsourced insurance authorization services are a practical option for physicians to standardize in-office processes for handling prior authorizations, obtain prior approval quickly, and get paid for services provided.
An Overview of the Prior Authorization Process
For medication prior authorization, the process typically starts when the physician prescribes a specific drug. When this is received by the pharmacy, the pharmacist will verify and validate if the prescription requires PA. Once confirmed, the pharmacy will contact the physician who prescribed the medication and inform the provider that the insurance company requires a PA. At this stage, the patient can either opt to wait for coverage approval from the insurance company or pay for full cost of the prescription themselves.
The physician will contact the insurance company and submit a formal authorization request according to the plan’s guidelines, along with the necessary forms. The submitted form must support the need for medical necessity with clinical documentation of the requested medication for approval. This can be initiated via phone, fax, email or automated message. The insurance company may also require the patient to complete some paperwork or sign some forms. The company will review the request and may either authorize the drug or refuse to cover it.
Why Does Prescription Require Prior Authorization?
Health insurers use prior authorization for certain medications to evaluate the medical necessity and cost-effectiveness of the prescription. The intention of pre-authorization is to ensure that the prescription aligns with the medical evidence-based guidelines to improve patient outcomes. Particularly highly expensive or specialty drugs necessitate strict evaluation to ensure no other lower cost alternate prescription exists that is equally effective. They also promote patient safety by ensuring the prescribed drug has no adverse health effect or risks for abuse.
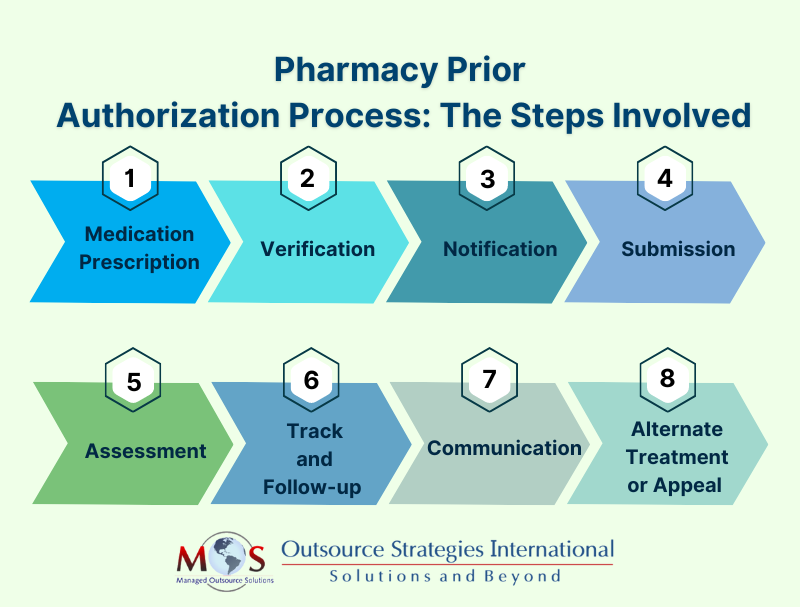
A Step-By-Step Guide to the Pharmacy Prior Authorization Process
- Medication prescription: The physician examines the patient’s health condition and orders the appropriate medication or prescription drug for the patient.
- Verification: The pharmacist receives the order for a prescription and verifies PA with the patient’s health insurance plan to determine the prior authorization requirement for the prescription.
- Notification: The pharmacist notifies the prescribing physician’s office regarding the pre-authorization status of the prescription.
- Submission: The physician or their staff begin the prior authorization process by filling out the pre-authorization form provided by the insurance company. The request should contain all the necessary clinical documentation about the patient to justify the medical necessity of the prescription.
- Assessment: The health insurance company receives the request for the approval of pre-authorization and reviews the form meticulously to ensure the prescription is medically necessary and the availability of any alternate, less expensive prescription. The insurer has their own medical experts and decides the outcome based on their evaluation. They may either consent, reject or ask for additional information.
- Track and follow-up: The physician’s office should maintain a record of the submission and a strict follow-up schedule to stay in contact with the insurance company to track progress.
- Communication: The insurance provider will convey their decision about the request to the physician and patient.
- Alternate treatment or appeal: If pre-authorization is obtained, then the pharmacist can supply the prescription to the patient. If denied, the physician will either discuss alternate options with the patient or file for an appeal.
Our pre- authorization services optimize operations and secure timely approvals with reduced risk of denials!
Tips for Improving the Pre-Authorization Process
Although it is not possible to manage every aspect of the pre-authorization process, healthcare providers can expedite the process by following the tips mentioned below:
Verification
Before prescribing a medication, especially certain expensive drugs, verify with the patient’s health plan to check if pre-authorization request is needed. This helps to save time and resources by accessing prior authorization status information beforehand. Developing a standard verification process streamlines operational efficiency to collect all the required patient clinical data, such as diagnosis, justification for the medication, and the availability of other alternatives.
Implement automation
Manual pre-authorization paperwork is a time-consuming process that is prone to human error or incomplete information about the prescription. Mitigate these concerns by automating the pre-authorization system with the existing EHR system to accelerate the process. Automated systems have benefits such as:
- An automated system can reduce the time lag involved in contacting the insurers for paperwork by providing real-time access to pre-authorization information for medications.
- Streamlines the entire administrative process by collecting and storing accurate patient information, thereby minimizing time, resources, and potential mistakes.
- Allows timely and automatic alerts to track the progress of the pre-authorization requests.
Employ a specialized team
Many practices delegate this task to office staff, who may not be familiar with all the pre-authorization requirements, which reduces their productivity and may cause costly administrative errors. So, to avoid this lapse, consider hiring a specialized team dedicated to providing insurance verification and pre-authorization services. This greatly enhances the efficiency of your medical billing process and minimizes the risk of errors. However, managing an in-house team might not be ideal as the resources needed for finding and hiring quality staff are challenging. As insurance verification and pre-authorization is an important part of the medical billing process, you may consider outsourcing to a medical billing company to handle your PA process effectively for timely approvals and prompt payments.
Mastering the pharmacy pre-authorization process is crucial for optimal patient care and reduced administrative burden. Delays in pharmacy PA approval could hinder patient care with postponed treatment and potential health concerns. An efficient, standardized and optimized pharmacy PA process is vital for rendering excellent patient care and securing reimbursement for your practice.