Systemic lupus erythematosus (SLE) is a chronic autoimmune disease that affects multiple organ systems and can present with a wide range of symptoms. For healthcare providers and medical coders, correctly reporting SLE using the appropriate ICD-10 codes is essential for ensuring accurate documentation, streamlined billing, and regulatory compliance. Due to the complexity of this condition and the specificity required by coding systems, understanding ICD-10 coding for systemic lupus erythematosus is vital for accurate documentation. In this post, we explore essential tips for accurate ICD-10 coding of autoimmune disorders like lupus to ensure proper documentation, compliance, and reimbursement.
Understanding Systemic Lupus Erythematosus (SLE)
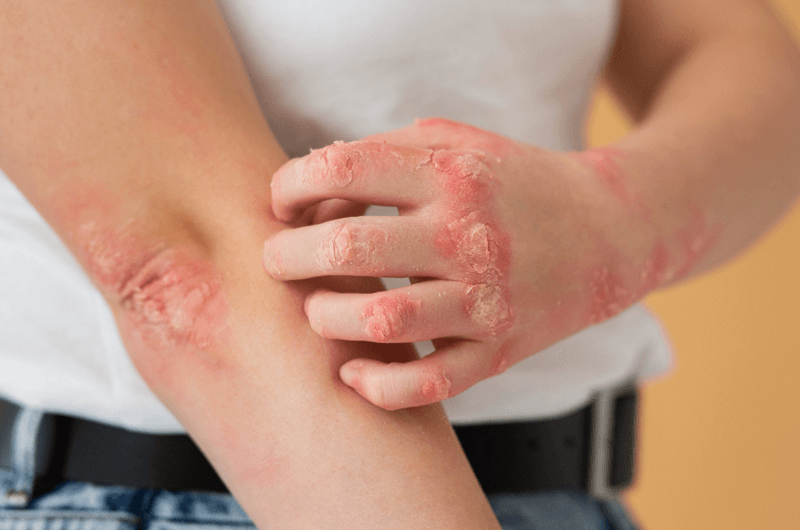
SLE is a complex autoimmune condition where the immune system mistakenly attacks healthy tissue. It commonly impacts the skin, joints, kidneys, heart, lungs, blood vessels, and nervous system. Symptoms can range from fatigue, rashes, and joint pain to life-threatening complications like kidney failure or myocarditis. Because of the multi-organ nature of the disease and its variable presentation, SLE must be clearly and precisely documented to ensure correct ICD-10 classification.
ICD-10 Coding for Systemic Lupus Erythematosus: Key Codes to Know
The ICD-10-CM system includes a dedicated set of codes under category M32, which specifically addresses SLE and its associated manifestations. Here are the most relevant codes:
- M32 Systemic lupus erythematosus (SLE)
- M32.0 Drug-induced systemic lupus erythematosus
- M32.1 Systemic lupus erythematosus with organ or system involvement
- M32.10 Systemic lupus erythematosus, organ or system involvement unspecified
- M32.11 Endocarditis in systemic lupus erythematosus
- M32.12 Pericarditis in systemic lupus erythematosus
- M32.13 Lung involvement in systemic lupus erythematosus
- M32.14 Glomerular disease in systemic lupus erythematosus
- M32.15 Tubulo-interstitial nephropathy in systemic lupus erythematosus
- M32.19 Other organ or system involvement in systemic lupus erythematosus
- M32.8 Other forms of systemic lupus erythematosus
- M32.9 Systemic lupus erythematosus, unspecified
Choosing the correct code depends on the specific organ involvement documented in the patient’s record. This makes it crucial for providers to detail all symptoms, affected systems, and diagnostic findings.
Medical Coding Best Practices for Lupus
When it comes to SLE medical coding, precision and documentation are everything. Here are some best practices for accurately coding systemic lupus using ICD-10:
- Document Specific Organ Involvement: Avoid using unspecified codes when possible. Clearly state if the patient has nephritis, pericarditis, or other organ manifestations related to lupus. This determines whether M32.14 (glomerular disease) or another sub code should be used.
- Differentiate Drug-Induced Lupus: SLE that arises due to certain medications (e.g., hydralazine, procainamide) must be coded with M32.0, which denotes drug-induced lupus.
- Include Secondary Diagnoses Where Applicable: SLE is often accompanied by anemia, hypertension, or infections. These should be captured as additional diagnosis codes to present a complete picture.
- Clarify Active vs. Historical SLE: Coders should ensure the provider has indicated whether the lupus is active or in remission, as this may affect documentation and payer guidelines.
- Verify Diagnostic Evidence: Coders should confirm that laboratory tests and physician documentation support the lupus diagnosis – especially in new cases or those involving a specific organ.
Ensure Coding Accuracy for Complex Autoimmune Cases.
Avoid claim denials and compliance risks with expert support in ICD-10 coding for systemic lupus erythematosus.
Tips for Accurate ICD-10 Coding of Lupus and Other Autoimmune Disorders
Accurate coding not only helps with reimbursement but also improves quality reporting. Here are some tips tailored for lupus and other autoimmune conditions:
- Use the full ICD-10 code including all required characters – do not stop at the category level (e.g., “M32”).
- Avoid unspecified codes like M32.9 unless documentation is truly incomplete or nonspecific.
- Audit medical records for key terms such as “lupus nephritis,” “serositis,” “malar rash,” or “ANA positive,” which can indicate specific complications.
- Stay updated on payer requirements, as some insurers require additional modifiers or supporting documentation for lupus-related treatments.
- Train healthcare providers on how to clearly document disease manifestations and treatment responses.
The Role of Medical Coding Outsourcing
As autoimmune diseases like lupus involve layered and evolving documentation, many healthcare practices benefit from medical coding outsourcing. Here’s how outsourcing supports better coding for conditions like SLE:
- Specialized coders familiar with autoimmune conditions and complex ICD-10 coding rules ensure accuracy.
- Reduced error rates, improving claim acceptance and reducing reimbursement delays.
- Faster turnaround with dedicated teams managing coding backlogs.
- Audit readiness, as outsourced partners often implement internal quality checks.
Medical coding outsourcing partners can also provide access to certified coders who stay current with annual ICD-10 updates, helping practices maintain compliance and reduce revenue cycle risks.
ICD-10 Coding for SLE: Key Takeaways
- Use M32.1 series when lupus involves specific organs (e.g., M32.14 for lupus nephritis).
- Select M32.0 if the lupus is drug-induced.
- Apply M32.9 only if no organ/system involvement is documented.
- Always code additional conditions such as hypertension, anemia, or infections.
Systemic lupus erythematosus is a highly variable autoimmune disease that requires nuanced documentation and coding. Accurate ICD-10 coding for systemic lupus erythematosus ensures appropriate reimbursement, better patient data tracking, and improved clinical outcomes. Leveraging outsourced medical coding services is a practical option for physicians to ensure coding best practices for lupus, navigate the complexities of SLE reporting with confidence, ensure compliance, and improve their revenue cycle.
Need Help Navigating ICD-10 Coding for SLE?
For reliable medical coding outsourcing services