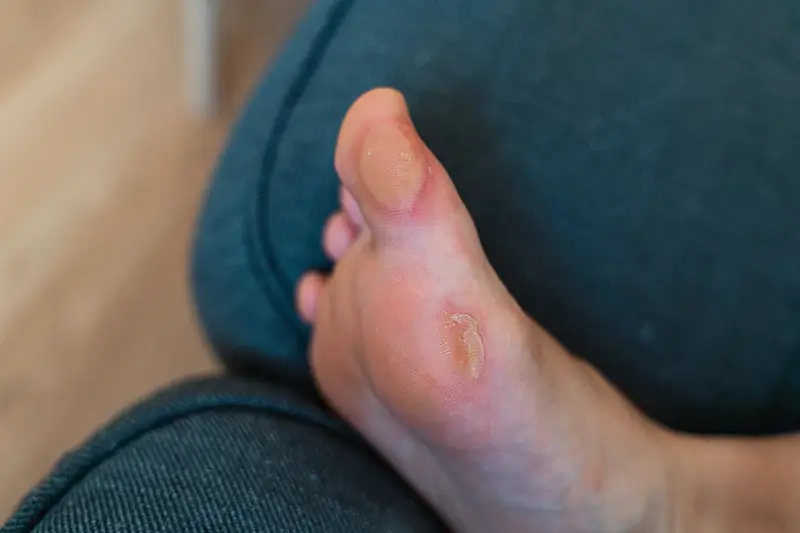
A common problem many people experience, an ulcer is an area of full-thickness skin breakdown. In simple terms, it is a break in the skin, which allows air and bacteria to get into the underlying tissues. The condition is usually caused by an injury (often a minor one) that breaks down the skin and in most cases these injuries will heal up without difficulty within a week or two. However, when the skin injuries do not heal and the breakdown increases, the ulcer becomes chronic. If the ulcer is not healing due to poor blood circulation, it is called arterial ulcer. Also referred to as ischemic ulcers, the condition develops due to inadequate supply of blood to the affected area (ischaemia).The condition is generally caused by the caused by poor perfusion (delivery of nutrient-rich blood) to the lower extremities. The overlying skin and tissues are deprived of oxygen, thus killing these tissues and causing the area to form an open wound. In addition, the lack of blood supply can result in minor scrapes or cuts failing to heal and eventually causing ulcers. Most commonly occurring in the lower legs and feet, arterial ulcers if left untreated can become acute or chronic. In most cases, untreated ulcers are prone to serious complications, including infection, tissue necrosis, and in extreme cases amputation of the affected limb. Treatment for the condition involves prescribing antibiotics. However, in some cases, treating the infection alone will not heal the ulcer. For non-healing, painful ulcers, treatment is required to improve the blood supply as with better blood circulation the pain improves quickly and the ulcer can start to heal. Coding skin ulcers is complex as the condition involves different phases of symptoms which can range from mild to severe. Outsourcing medical billing and coding would be a practical solution for timely claim filing and correct reimbursement.
Apart from blocked arteries, other related causes include – diabetes, high blood pressure and cholesterol, kidney failure, atherosclerosis, or thickening of the arteries, vasculitis, obesity, rheumatoid arthritis, clotting and circulation disorders, age and smoking.
Symptoms and Risk Factors
Arterial ulcers often occur on the foot, around the ankle, heels, or toes and the lower leg and have a “punched out” appearance. These can form in other areas as well. Chronic pain and swelling are one of the most common symptoms associated with the condition. The pain can become worse at night. Other related symptoms of arterial ulcers include –
- Red, yellow, or black sores
- Tight, hairless skin
- Reddening of legs (when dangled and turns pale when elevated)
- No bleeding
- Leg pain at night
- Deep wound
- Affected area is cold to touch from minimal blood circulation
- Delayed capillary return in the affected extremity
How Are Arterial Ulcers Diagnosed and Treated?
The underlying cause for an arterial ulcer is diagnosed by performing a detailed patient history evaluation and a careful physical examination. Physicians may perform a wide range of diagnostic imaging tests like – Ankle Brachial Pressure Index (ABPI), Transcutaneous Oximetry, Buerger test, Absolute toe systolic pressure, Arterial Doppler studies and Capillary refill time to correctly identify the causes and intensity of symptoms.
Before suggesting any treatment options, physicians need to identify the underlying cause. Ulcers can be generally treated with proper care and antibiotics. However, correct diagnosis of the underlying causes can ensure that the condition heals properly and does not reoccur. Primary treatment modality focuses on increasing blood circulation to the affected area and reducing the pain. Using antibiotics can help reduce the intensity of symptoms, but won’t heal the ulcer completely.
The primary goal behind the treatment for arterial ulcers is to address the relevant factors contributing to arterial insufficiency and subsequent ulcer development. These include – managing wound infections through prescription medications, incorporating certain lifestyle changes and proper wound care. Keeping the ulcer area of the skin clean and moist by regularly changing wound dressings and physical or chemical debridement (removing areas of dead tissue) is vital. It is important to discuss with the physicians on how often patients need to change the bandages. In addition, incorporating key lifestyle changes like stopping the habit of smoking and changing the diet patterns help reduce blood lipid and control or manage cholesterol and blood sugar levels. Treating the underlying cause with antibiotics can help reduce symptoms, but it won’t heal the ulcer completely. In addition to antibiotics, physicians may recommend surgical options to restore blood flow to tissues and organs. In severe cases of arterial ulcers, surgical intervention may be recommended. Skin grafting is an important surgical technique wherein a thin piece of skin is taken from another site, (usually the upper thigh) and placed over the wound. A skin flap is an alternative way to cover the wound. The surgical revascularization of a limb is another option that aims to restore blood flow either by bypassing or angioplasty (re-opening) of narrowed vessels. This improves the healing of an ischemic ulcer by restoring oxygen and nutrient supply to the tissues.
Treatment procedures administered by general physicians or other specialists must be documented using the right medical codes. Medical billing services offered by reputable billing and coding companies ensure this so that accurate claim submissions are done. ICD-10 diagnosis codes for arterial ulcers include –
- I70 Atherosclerosis
- I70.0 Atherosclerosis of aorta
- I70.1 Atherosclerosis of renal artery
- I70.2 Atherosclerosis of native arteries of the extremities
- I70.20 Unspecified atherosclerosis of native arteries of extremities
- I70.201 …… right leg
- I70.202 …… left leg
- I70.203 …… bilateral legs
- I70.208 …… other extremity
- I70.209 …… unspecified extremity
- I70.21 Atherosclerosis of native arteries of extremities with intermittent claudication
- I70.211 …… right leg
- I70.212 …… left leg
- I70.213 …… bilateral legs
- I70.218 …… other extremity
- I70.219 …… unspecified extremity
- I70.22 Atherosclerosis of native arteries of extremities with rest pain
- I70.221 …… right leg
- I70.222 …… left leg
- I70.223 …… bilateral legs
- I70.228 …… other extremity
- I70.229 …… unspecified extremity
- I70.23 Atherosclerosis of native arteries of right leg with ulceration
- I70.231 …… of thigh
- I70.232 …… of calf
- I70.233 …… of ankle
- I70.234 …… of heel and midfoot
- I70.235 …… of other part of foot
- I70.238 …… of other part of lower leg
- I70.239 …… of unspecified site
- I70.24 Atherosclerosis of native arteries of left leg with ulceration
- I70.241 …… of thigh
- I70.242 …… of calf
- I70.243 …… of ankle
- I70.244 …… of heel and midfoot
- I70.245 …… of other part of foot
- I70.248 …… of other part of lower leg
- I70.249 …… of unspecified site
- I70.25 Atherosclerosis of native arteries of other extremities with ulceration
- I70.26 Atherosclerosis of native arteries of extremities with gangrene
- I70.261 …… right leg
- I70.262 …… left leg
- I70.263 …… bilateral legs
- I70.268 …… other extremity
- I70.269 …… unspecified extremity
- I70.29 Other atherosclerosis of native arteries of extremities
- I70.291 …… right leg
- I70.292 …… left leg
- I70.293 …… bilateral legs
- I70.298 …… other extremity
- I70.299 …… unspecified extremity
If left untreated, these ulcers can cause serious complications like infections and in extreme cases lead to amputation of the affected limb. Patients, who experience irregular symptoms, wounds or notice pain in the lower extremities, must seek immediate medical attention as these wounds or symptoms could be indicators of a more serious condition.
Importance of Proper Wound Care
Wound Care is considered medically necessary for arterial insufficiency related wounds, as such chronic wounds take quite a long time to heal. Standard wound care includes keeping the ulcer clean and moist by regularly changing wound dressings, compression wrapping, pressure reduction techniques, removing dead tissues and treating wound infection. Wound care treatment modalities for arterial ulcers may include Extracellular matrix replacement therapy, Electrical Stimulation and Electromagnetic Therapy, Negative Pressure Device therapy or Ultrasound Therapy. Coverage for each treatment may differ with insurers. Most treatments are reimbursable, only if they are proven to be medically necessary. For instance, the use of Electrical Stimulation (ES) and electromagnetic therapy is considered medically necessary only after 30 days of standard wound care has failed. At the same time, this therapy is NOT considered medically necessary in the following circumstances – As an initial treatment modality, measurable signs of healing have not been demonstrated within a 30-day period of treatment, or if treatment is used in an unsupervised setting (home use).
How Important is Insurance Verification and Prior Authorization in Wound Care?
Since arterial ulcers tend to be slow-healing wounds, they require long-term care in a hospital or other healthcare facility. This makes insurance verification important for long-term care, and for hospitals to receive on-time reimbursement. Timely and accurate insurance eligibility verification and authorization is vital to such providers. Not verifying insurance eligibility on time may impact revenue reimbursement. Prior authorization from payers is also required to obtain approval for certain wound care treatments. Verifying patient’s insurance before appointment provides diverse benefits such as submitting clean claims, preventing claim denials, avoiding delays in payment, improving cash collection, minimizing bad debt, and increasing patient satisfaction.
Wound care clinics and long-term care practices must make sure to verify the patient’s insurance coverage before or during the initial consultation itself and if the insurance provider requires co-pay, verify this payment at each visit. Insurance details that need to be verified include effective dates of insurance coverage, payable benefits, co-insurance, deductible amount, status of patient’s insurance policy, pre-authorizations, referrals, mailing address and DME reimbursement. To make the insurance verification and authorization process easy with patients, practices must make sure that each staff, mainly the front office, is familiar with the documentation requirements and can print out the latest medical policy on the procedure with an authorization request for the patient. Wound care insurance verification and prior authorization services provided by an experienced medical billing company would be of great support.
Healthcare providers need to be up to date about the related diagnosis and procedures codes to report arterial ulcers. Outsourced billing services offered by AAPC-certified billers and coders can help physicians optimize reimbursement for the services they offer.