In the healthcare sector, successful patient eligibility verification facilitates smoother financial transactions and enhances patient satisfaction. Coverage validation is an important stage in healthcare revenue cycle management, encompassing the confirmation of a patient’s insurance coverage and benefits. Beyond facilitating continuous billing and reimbursement, benefit verification serves as a preventive measure against claim denials, mitigating the financial strain on both patients and healthcare organizations. Professional insurance verification services are a viable option for healthcare providers to manage the process, collect payments from insurance companies and patients proactively, and prevent delays in cash realization.
Let us check out the main components of effective insurance verification.


Ready to streamline your revenue cycle?
Experience the efficiency of our cutting-edge insurance verification services.
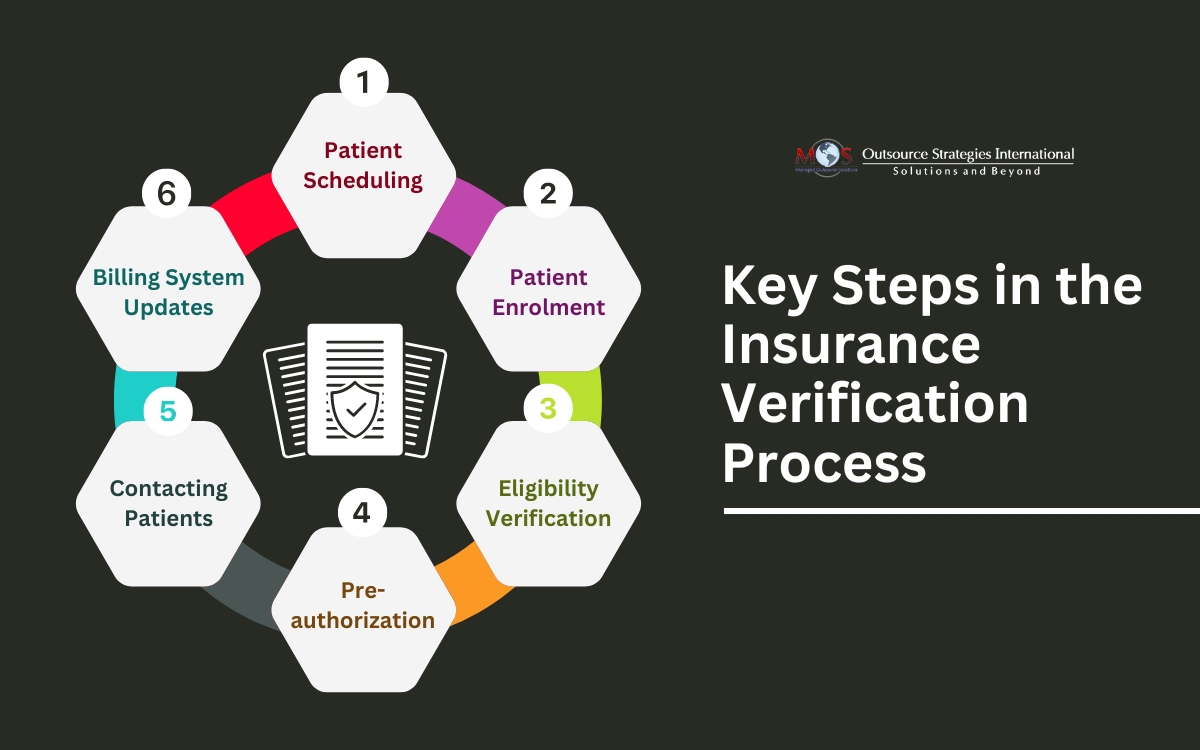
Steps in the Insurance Verification Process
The key elements of successful medical insurance eligibility checks are as follows:
Accurate patient information gathering: The foundation of this verification process lies in collecting precise patient details. Providers must ensure accurate recording of the patient’s personal information, including name, date of birth, address, and contact details. Any discrepancies at this stage can lead to errors throughout the process.
Thorough policy verification: Comprehensive benefits verification involves confirming the patient’s insurance coverage details, including policy number, coverage start and end dates, and any specific limitations or restrictions. Confirming the type of insurance plan and its benefits ensures that the provider has a clear understanding of what services are covered.
Real-time access to payer information: Using technology for real-time access to payer databases is crucial. This allows providers to verify insurance information instantly and ensures that the data is up-to-date. EHR integration with payer systems facilitates efficient real-time eligibility checks and reduces the risk of relying on outdated or inaccurate information.
Verification of co-pay and deductible information: Understanding patient financial responsibility is essential for both providers and patients. Verifying co-pay and deductible information helps in communicating potential out-of-pocket costs to patients upfront, preventing surprises and fostering transparent financial transactions.
Integration with practice management systems: Seamless integration with practice management systems enhances workflow efficiency. When insurance verification is integrated into the provider’s existing systems, it minimizes the need for duplicate data entry, reduces administrative burden, and promotes consistency in records.
Clear communication with patients: Effective communication with patients regarding their insurance coverage is vital. Providers should explain the verification process, outline covered services, and inform patients of any financial responsibility. Transparent communication fosters patient trust and helps in managing expectations.
Staff training and education: Regular training sessions ensure that staff members are familiar with the latest updates in insurance policies, billing codes, and any changes in regulations that may impact the verification process.
Outsourcing insurance verification can help avoid the in-house burden of hiring, training and managing staff for this critical front-end revenue cycle management task. It ensures access to professionals with in-depth knowledge and experience in navigating the complexities of insurance plans, policies, and procedures.
Hope you’ve listened to our podcast:
By embracing real-time technology, prioritizing accuracy, and fostering clear communication, healthcare providers can enhance patient satisfaction, streamline administrative processes, and ultimately optimize their financial performance.
Outsourcing can overcome the common challenges in insurance verification. It is important for healthcare providers to choose a reliable insurance authorization and verification company that has a comprehensive understanding of insurance policies and utilizes advanced technology tools, ensuring real-time access to updated payer information. Providers should partner with a company that offers seamless integration with existing practice management systems, minimizing manual errors and streamlining workflows.


Take control of your billing challenges!
For more information about our insurance verification services.




