Evaluation and Management (E/M) codes are the most common professional services that a medical billing and coding company helps physicians report on claims. The rules for documenting these services are periodically re-evaluated and revised to improve patient care and reduce administrative burden. On January 1, 2021, several office and outpatient E/M coding changes came into effect, which includes major changes for prolonged Evaluation & Management (E/M) codes. New codes have been added to bill for prolonged services, involving direct and indirect patient contact provided in various settings beyond the usual evaluation and management services.
Role of Time in Selection of E/M Service Level
Time plays a major role in the selection of the most appropriate level of E/M services. Beginning with CPT 2021, except for 99211 (office or other outpatient visit for the E&M of an established patient that may not require the presence of a physician), time alone may be used to select the appropriate code level for the office or other outpatient E/M services codes (99202, 99203, 99204, 99205, 99212, 99213, 99214, 99215).
As time is used differently in different categories of services, the American Medical Association (AMA) emphasizes that instructions for each category should be reviewed. When time is used for reporting E/M services codes, the appropriate level of services is selected using the time defined in the service descriptors. These guidelines apply for E/M services that involve a face-to-face encounter with the physician or other qualified health care professional. When prolonged time occurs, the appropriate prolonged services code should be reported.
The AMA lists the following activities as included in physician/other qualified health care professional time:
- preparing to see the patient (e.g., review of tests)
- obtaining and/or reviewing separately obtained history
- performing a medically appropriate examination and/or evaluation
- counseling and educating the patient/family/caregiver
- ordering medications, tests, or procedures
- referring and communicating with other health care professionals (when not separately reported)
- documenting clinical information in the electronic or other health record
- independently interpreting results (not separately reported) and communicating results to the patient/ family/caregiver
- care coordination (not separately reported)
The AMA instructs: Do not count time spent on the following:
- the performance of other services that are reported separately
- travel
- teaching that is general and not limited to discussion that is required for the management of a specific patient
New Prolonged Service Codes
There are two new prolonged service codes for 2021 that are specific to E/M codes 99205 and 99215:
- CPT code 99417 can be reported for each 15 minutes of prolonged care performed on the same day beyond the maximum time listed for E/M codes 99205 and 99215.99417 – Prolonged office or other outpatient evaluation and management service(s) beyond the minimum required time of the primary procedure which has been selected using total time, requiring total time with or without direct patient contact beyond the usual service, on the date of the primary service, each 15 minutes of total time (List separately in addition to codes 99205, 99215 for office or other outpatient Evaluation and Management services)
- HCPCS code G2212 was created by the Centers for Medicare and Medicaid Services (CMS) is also intended for reporting prolonged services specific to 99205 and 99215.G2212 – Prolonged office or other outpatient evaluation and management service(s) beyond the maximum required time of the primary procedure which has been selected using total time on the date of the primary service; each additional 15 minutes by the physician or qualified healthcare professional, with or without direct patient contact (List separately in addition to CPT codes 99205, 99215 for office or other outpatient evaluation and management services)
Prolonged Services Reporting – Points to Note
- Both CPT code 99417 and HCPCS code G2212 may only be reported in conjunction with level 5 visit codes 99205 or 99215, if the codes were selected based on the time alone and not medical decision making.
- The payer’s policy should be checked for appropriate reporting guidelines:
- Report CPT code 99417 when billing payers other than Medicare. This code, should only be billed with 99205 or 99215 and represents an additional 15 minutes beyond the minimum time of the office visit code. It can be billed in multiple units for each additional 15 minutes of time. Additional time less than 15 minutes should not be reported.
- Code G2212 is specific to Medicare and payers who follow Medicare guidelines. It should be reported for each additional 15 minutes of prolonged service beyond the maximum time for CPT Codes 99205 or 99215
The following table shows the total time required for reporting codes G2212 and 99417:
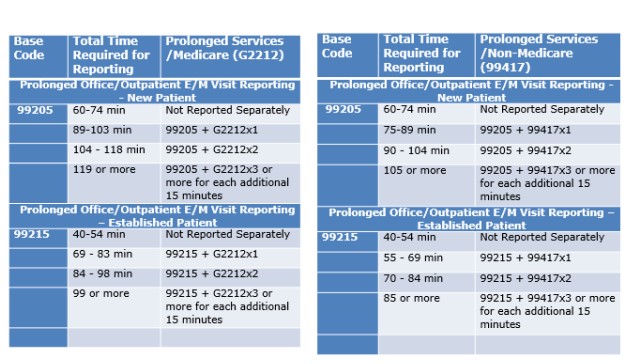
Reliable medical billing and coding service providers keep track of changes in reporting of E/M services and can help practices ensure accurate reporting of the new codes to comply with payer guidelines.




