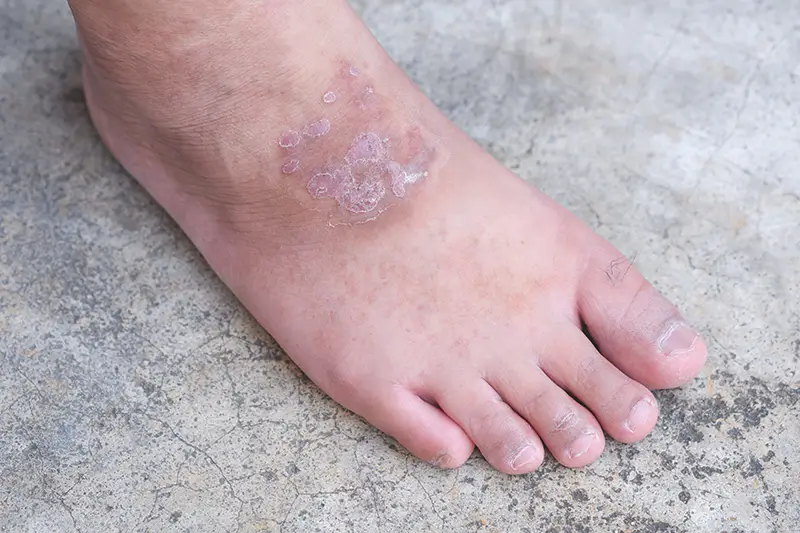
A chronic, lifestyle disorder affecting millions of people worldwide, diabetes involves high blood sugar levels, due to a lack of insulin or insulin not working properly. The condition can affect many parts of the body, including the skin. In fact, skin problems are in most cases the first warning signs that a person has diabetes. It is estimated that about one-third of people with diabetes will develop skin problems either related to or influenced by the condition. Diabetic blisters are one such rare skin disorder that tends to occur in people who do not control blood sugar well.
Also known as bullosis diabeticorum or diabetic bullae, these are painless and normally heal on their own without leaving scars. Proper management of blood glucose level can help prevent this skin problem associated with diabetes. Often, diagnosing diabetes-related skin conditions can be complex. When it comes to reporting diagnoses, diabetologists or other physicians can always rely on experienced medical billing companies that can easily and correctly manage the coding and claim submission processes.
Causes and Appearance of Diabetic Blisters
Diabetic blisters are twice as likely to be found in men than in women. The exact factors that tend to cause diabetic blisters is unknown. However, several factors like – reduced blood circulation, shoes that do not fit correctly, fungal infections (Candida albicans) and other injury or irritation in the feet or hands – can play an active role in the development of blisters. This skin problem often occurs in people who have severe diabetes and diabetic neuropathy. Peripheral artery disease and sensitivity to ultraviolet (UV) light is also thought to play a role.
As mentioned above, diabetic blisters often develop in people who do not control their diabetes correctly for several years. Despite this, some people may find that these blisters are the initial symptom they experience as a result of diabetes or even pre-diabetes. These blisters most often appear on the legs, feet, and toes. Less frequently, they show up on the hands, fingers, and arms. Blisters are usually clear bumps that have an irregular shape. They are painless and tend to heal on their own without treatment. Other symptoms include –
- Appearance can be up to 6 inches across
- Occurs in clusters or less commonly, occurs as a single lesion
- Filled with a clear fluid
- Causes an itching sensation
- Appears like a mark that occurs when a person suffers a burn (only without the pain)
In most cases, the skin around diabetic blisters will usually look healthy and will heal on its own, but there is a risk of secondary infection. However, if certain symptoms like – redness/swelling/ pain around the blister, warmth radiating from the lesion and fever appears, it is important to contact the physician immediately.
Treatment for Diabetic Blisters
Considering the risk of infection and ulceration that diabetes presents, patients need to consult a dermatologist during an initial stage to rule out more serious skin conditions. Diabetic blisters usually heal in two to five weeks without intervention. One of the main ways to treat this condition is to prevent the occurrence or chances of infection. The fluid in the blisters is sterile. One of the primary ways to prevent infection is to avoid puncturing or bursting the blisters (even though they are large). If the lesion is large, physicians may drain the fluid to keep the skin intact as a covering for the wound, if the blister ruptures accidentally, which is quite rare. Treatment for large, persistent, painful, or inflamed blisters involves a combination of methods like – saline compresses (that help relieve itching and irritation), bandaging, and aspiration. Topical antibiotics or steroids may also be prescribed to protect blisters from further injury.
ICD-10 Codes for Diabetic Blisters
- S90.82 – Blister (nonthermal) of foot
- S90.821 – Blister (nonthermal), right foot
- S90.821A – Blister (nonthermal), right foot, initial encounter
- S90.821D – Blister (nonthermal), right foot, subsequent encounter
- S90.821S – Blister (nonthermal), right foot, sequela
- S90.822 – Blister (nonthermal), left foot
- S90.822A – Blister (nonthermal), left foot, initial encounter
- S90.822D – Blister (nonthermal), left foot, subsequent encounter
- S90.822S – Blister (nonthermal), left foot, sequela
- S90.829 – Blister (nonthermal), unspecified foot
- S90.829A – Blister (nonthermal), unspecified foot, initial encounter
- S90.829D – Blister (nonthermal), unspecified foot, subsequent encounter
- S90.829S – Blister (nonthermal), unspecified foot, sequela
In most cases, keeping the blood sugar levels under control is one of the most important steps to prevent diabetic blisters. Consuming the correct medications and incorporating essential dietary and lifestyle changes can help in effective blood glucose control. People with diabetes need to closely monitor their skin health (particularly arms, hands, legs, and feet) to look for blisters and other skin conditions. In addition, limiting exposure to UV light, and using sunscreen when going outdoors is also important.
Healthcare providers need to be well-informed about the specific ICD-10 codes to report diabetes-related skin disorders. A reliable provider of medical coding services can help physicians with accurate claim submission for optimal reimbursement.