Diabetes is considered a fast-growing, chronic disease affecting millions of people across the globe. People with diabetes have high blood sugar levels, due to a lack of insulin or insulin not working properly. According to recent reports, more than 25 million people in the United States suffer from diabetes. It is estimated that the diabetes epidemic will escalate and by the end of 2050, one in three Americans will have diabetes. The condition can affect many parts of the body, including your skin. According to the American Diabetes Association (ADA), skin complications can be the initial warning signs of high blood sugar levels in people who remain undiagnosed. About one-third of people with diabetes will develop skin problems either related to or influenced by the condition. Most of these diabetes-related skin complications are harmless, but some can result in painful and persistent symptoms, which may require medical attention. The most effective treatment option for many diabetes-related skin conditions is effective blood sugar management. Proper control of your blood glucose level can help prevent diabetes-associated skin problems and many other symptoms from occurring in the first place. In other severe cases, however, a doctor may prescribe oral steroids, medicated creams, or another treatment. Diagnosing diabetes-related skin conditions can be complex. When it comes to reporting diagnoses, diabetologists or other physicians can always rely on experienced medical billing companies. Skilled medical coding service providers who have extensive knowledge about the codes and related guidelines can easily manage the coding and claim submission processes.
Let’s take a look at some of the common skin ailments triggered or worsened by diabetes and their ICD-10 codes –
Acanthnosis nigricans
This is a common skin pigmentation disorder characterized by areas of dark, velvety discoloration in body folds and creases. Notable signs of this condition are dark patches of skin with a thick, velvety texture. These patches may appear on skin folds and other areas, such as the neck, groin, armpits, elbows, knees, knuckles, palms and soles of feet. Acanthosis nigricans is not a disease; rather it is a symptom of another condition that may require medical attention. The skin problem usually strikes people who are overweight. While there is no cure for acanthosis nigricans, losing weight may improve the skin condition. Treatment is largely focused on addressing the condition that is causing it. However, if the condition is caused by medications or supplements, your doctor may suggest discontinuing them or recommend substitutes.
The ICD-10 code for Acanthosis nigricans is –
- L83 – Acanthosis nigricans
Vitiligo
Vitiligo is a disease that causes the loss of skin color in blotches. The condition occurs when the cells that produce melanin die or stop functioning. It can affect the skin on any part of the body and it may also affect the hair and inside of the mouth. Vitiligo can affect people of all skin types, but is most commonly seen in people with darker skin. Patchy loss of skin color is one of the initial symptoms of the condition. In most cases, the discoloration first shows on sun-exposed areas such as the hands, feet, arms, face and lips. Other related symptoms include – premature whitening or graying of the hair (on the scalp, eyelashes, eyebrows or beard), loss of color in the tissues that line the inside of your mouth and nose (mucous membranes), and loss of or change in color of the inner layer of the eyeball (retina). Treatment for vitiligo may restore color to the affected skin, but it does not prevent continued loss of skin color or a recurrence. Treatment options are medications, therapies (like psoralen and light therapy, de-pigmentation and surgery (like blister/skin grafting, micro-pigmentation) in severe cases.
The ICD-10 code to report vitiligo diagnosisis –
- L80 – Vitiligo
Necrobiosis lipoidica diabeticorum (NLD)
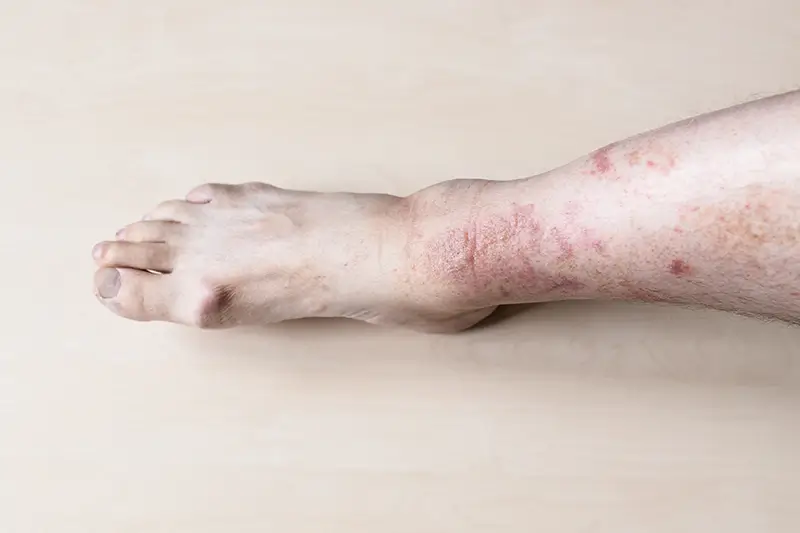
Necrobiosis lipoidica diabeticorum is a skin condition related to diabetes, which results in reddish brown areas of the skin, most commonly on the lower legs. The exact cause of this condition is unknown. But it is linked to blood vessel inflammation related to autoimmune factors. This damages proteins in the skin (collagen). Skin lesions occurring in the forearms are one of the most common symptoms. In some rare cases, these lesions can also occur on the stomach, face, scalp, palms, and soles of the feet. NLD is often very difficult to treat. Common treatment options include corticosteroid creams/injections, anti-inflammatory medications, medicines to improve blood flow, photo therapy and laser therapy. In severe cases, the lesions may be removed by surgery, followed by moving (grafting) skin from other parts of body to the operated area.
The ICD -10 code for NLD is –
- L92.1 – Necrobiosis lipoidica, not elsewhere classified
Eruptive xanthomatosis (EX)
Eruptive xanthomatosis is a skin condition that causes small, harmless yellow-red bumps (also known as eruptive xanthomas) to appear on the skin. These bumps are sometimes referred to as lesions, papules, plaques, or a rash. Severe insulin resistance (often associated with diabetes) can make it harder for the body to break down fats in the blood. This increases the level of fats in the blood, which can get deposited under the skin to form small bumps (lesions). EX is very common among people with poorly-controlled diabetes who have very high triglycerides and high cholesterol. EX causes a group of round little bumps, which look like a cluster of small, hard, raised spots. They are usually found on the back of your arms such as around your elbows and on the back of your thighs, buttocks, and legs. In some cases, they can also show up around your eyes and other areas like the stomach, neck, back, knees, scalp and face. These bumps cause symptoms like itching, pain, redness and oozing. Generally, EX bumps go away in a few weeks to months.
ICD-10 code is –
- E78.2 – Mixed hyperlipidemia
Diabetic blisters
Diabetic blisters typically occur in people who do not control blood sugar well. Blisters are usually clear bumps that have an irregular shape. They are painless and tend to heal on their own without treatment. These blisters most often appear on your legs, feet, and toes. Less frequently, they show up on the hands, fingers, and arms. This skin problem often occurs in people who have severe diabetes and diabetic neuropathy. Bringing your blood sugar level under control is one of the initial treatments for this skin condition. Diabetic blisters have high risk of infection and ulceration. One of the primary ways to prevent infection is to avoid puncturing or bursting the blisters. Blisters may be treated with antibiotic creams, steroidal creams and bandages to protect them from further injury.
Related ICD-10 codes include –
S90.82 – Blister (nonthermal) of foot
- S90.821 – Blister (nonthermal), right foot
- S90.821A – Blister (nonthermal), right foot, initial encounter
- S90.821D – Blister (nonthermal), right foot, subsequent encounter
- S90.821S – Blister (nonthermal), right foot, sequela
- S90.822 – Blister (nonthermal), left foot
- S90.822A – Blister (nonthermal), left foot, initial encounter
- S90.822D – Blister (nonthermal), left foot, subsequent encounter
- S90.822S – Blister (nonthermal), left foot, sequela
- S90.829 – Blister (nonthermal), unspecified foot
- S90.829A – Blister (nonthermal), unspecified foot, initial encounter
- S90.829D – Blister (nonthermal), unspecified foot, subsequent encounter
- S90.829S – Blister (nonthermal), unspecified foot, sequela
Granuloma annulare
Granuloma annulare is a skin condition that causes raised reddish or skin-colored bumps (lesions) that spread outwards in a ring pattern. Bumps often occur on the hands, fingers, and forearms. The National Organization for Rare Diseases (NORD) notes that granuloma annulare may be a complication of diabetes or shingles (herpes zoster), although it is unclear why the bumps develop. The lesions usually disappear on their own within two years without treatment. Treatment options include – Corticosteroid creams/ointments/injections, freezing, light therapy and other oral medications which help fade the bumps faster.
ICD-10 codes for Granuloma annulare include –
- L92 – Granulomatous disorders of skin and subcutaneous tissue
- L92.0 – Granuloma annulare
- L92.1 – Necrobiosis lipoidica, not elsewhere classified
- L92.2 – Granuloma faciale [eosinophilic granuloma of skin]
- L92.3 – Foreign body granuloma of the skin and subcutaneous tissue
- L92.8 – Other granulomatous disorders of the skin and subcutaneous tissue
- L92.9 – Granulomatous disorder of the skin and subcutaneous tissue, unspecified
Keeping your diabetes under control is one of the best ways to reduce the risk, severity and frequency of skin-related complications of diabetes. It is important to correctly follow your physician’s advice regarding nutrition, exercise, and medicine. Lifestyle tips for achieving and maintaining healthy blood sugar levels include – following a healthy diet, getting regular exercise, maintaining a healthy body weight and following the treatment plan, (including regular use of any medications as recommended by the physician). Attention to personal care and hygiene can help prevent these complications. Proper skin care also can help reduce your risk of skin-related problems. The National Institute of Diabetes and Digestive and Kidney Diseases recommend general measures to keep the skin healthy. These include – keeping the skin clean and dry, regularly monitoring the skin for sores, dry spots, and rashes, wearing cotton clothing and using moisturizers to hydrate the skin.
Healthcare providers need to be well-informed about the specific ICD-10 codes to report common diabetes-related skin disorders. A reliable medical billing and coding company can help physicians with accurate claim submission for optimal reimbursement.