21+
Years in the Industry
MedGenX uses DeepKnit AI to automate coding end-to-end with advanced algorithms, OCR/ICR, and predictive analytics. Built by certified coders and supported by human-in-the-loop review, this AI-powered software delivers compliant medical codes in seconds, which improves accuracy and productivity, captures revenue faster, and improves costs.
Key Features Engineered for High-Speed, Accurate Medical Coding
Designed for flexibility, MedGenX can be adapted to each organization’s unique workflows, specialties, and payer requirements, ensuring coding aligns with specific operational needs. Built-in quality control continuously detects discrepancies, delivering consistent, high-accuracy results while reducing denials and rework for reliable performance.
Comprehensive Code Coverage
Assigns ICD-10, CPT, HCPCS, CDT, and revenue codes automatically.
Specialty-Aware Intelligence
AI-driven Coding Logic
Coverage Policy Coding Support
Advanced AI Understanding
Human-in-the-Loop QA
Interactive Gap Resolution
Retrospective Audit Mode
Workflow Integration
Multi-Note Batch Coding
Continuous Learning Engine
Documentation Enhancement
MedGenX ensures HIPAA-compliant security using strong encryption to protect sensitive patient data.
Explore MedGenX’s Automated Medical Coding Features
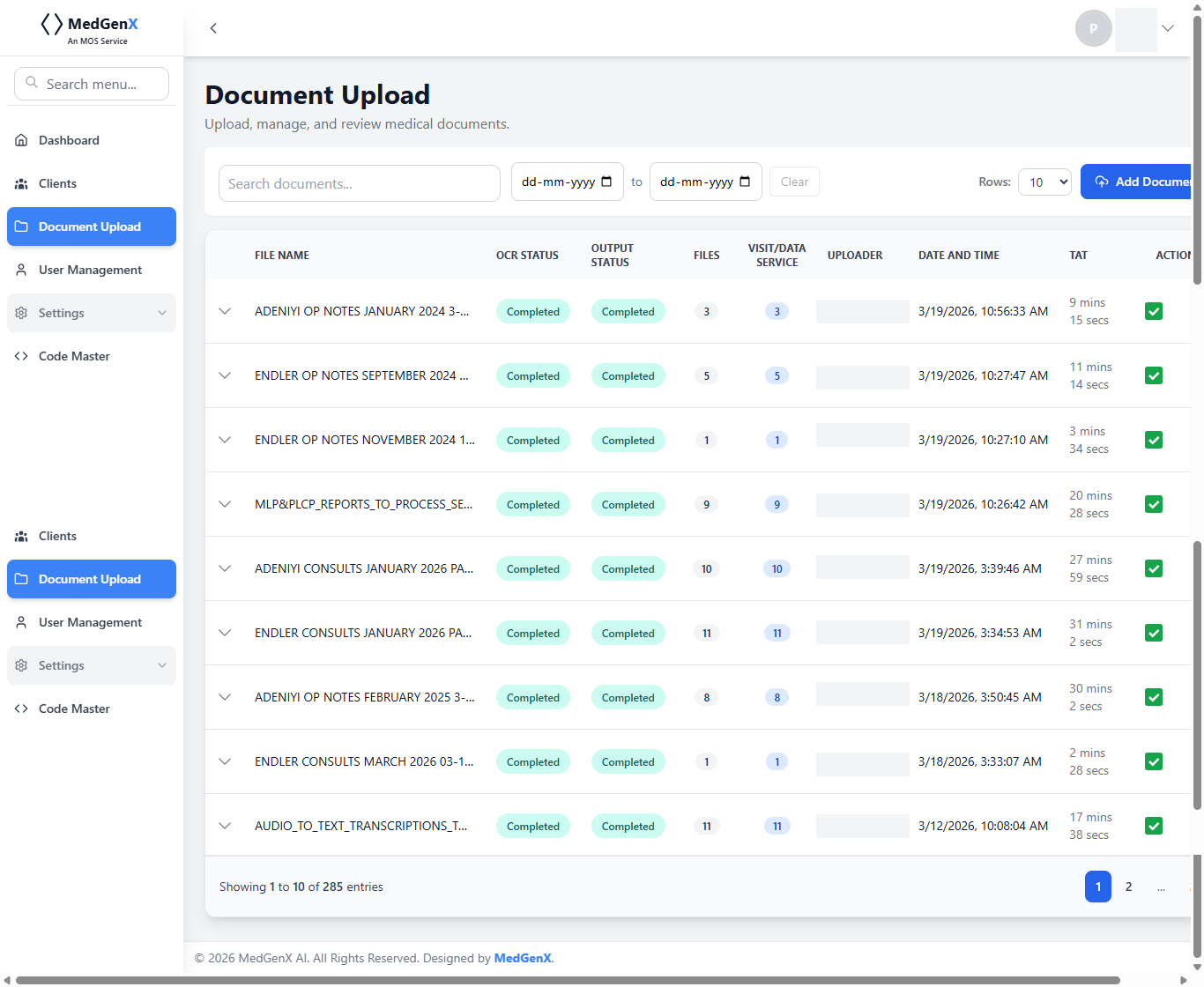
Access summaries, coding suggestions, and reports—all in one streamlined view.
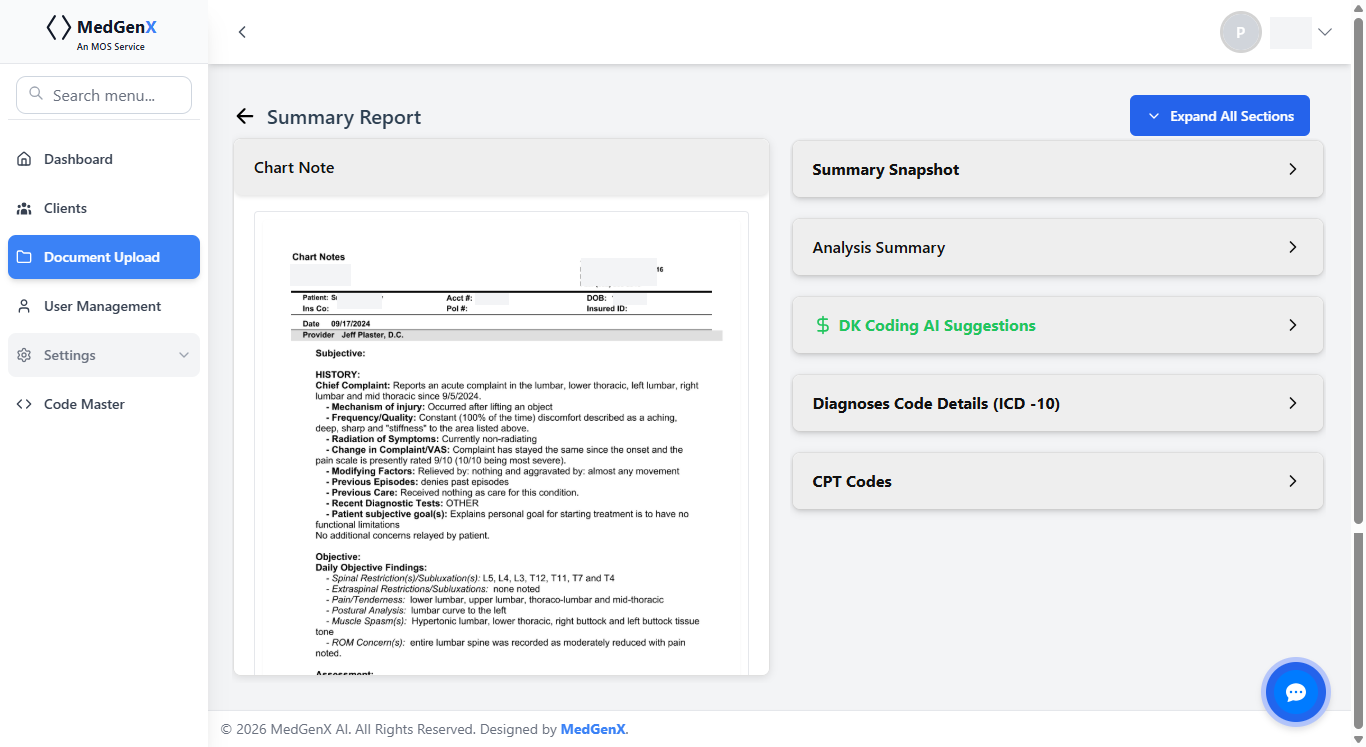
Extracts key procedural details from operative notes for precise documentation and coding.
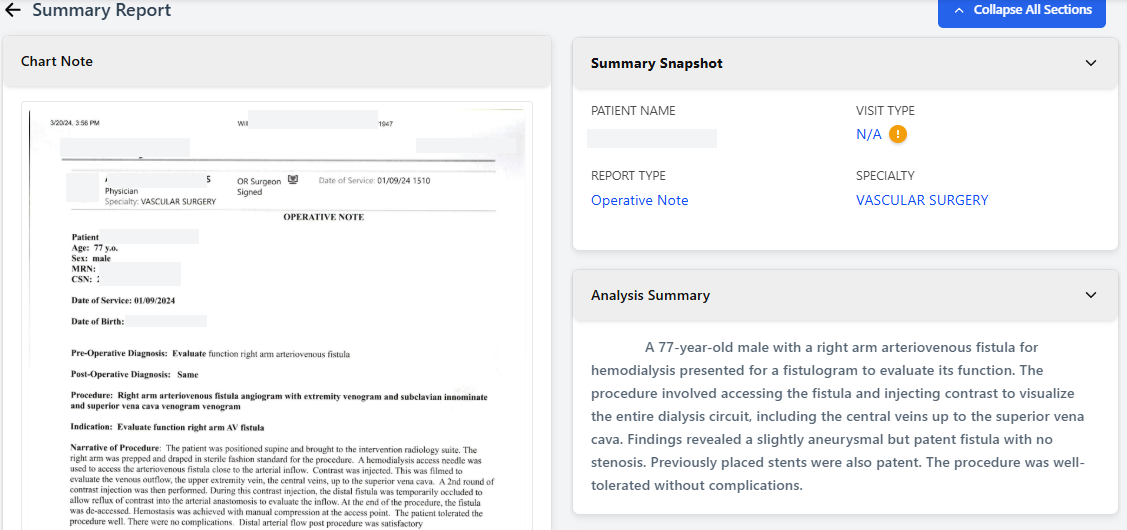
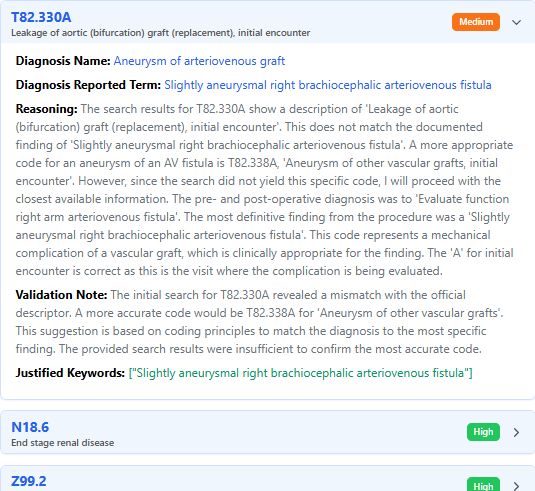
Flags inconsistencies and suggests documentation or coding improvements in real time.

MedGenX: Powering the Future of Faster, Smarter Medical Coding
By eliminating manual bottlenecks and optimizing workflows, MedGenX enables scalable, high-performance coding that supports faster claims, cleaner audits, and sustainable revenue growth.

Fast & Accurate
AI-powered coding with human review ensures accuracy and compliance across specialties in seconds.

Cost-Efficient
Handle high volumes, cut costs, and speed up claims for improved cash flow and fewer denials.

Reliable Automation
Avoid black-box risks with expert oversight, delivering consistent, audit-ready results that boost revenue.
Accuracy, Speed, and Compliance Built into Every Chart
How MedGenX Works:
1
End-to-End Automation
Upload a note – MedGenX delivers fully automated, complete coding in seconds.
2
Deep Clinical Understanding
Advanced NLP reads clinical context like an expert coder across all specialties.
Built-In Compliance
Automatic MDM logic, guideline checks, and payer rules ensure first-pass accuracy.
Coding Gap Analysis
AI flags ambiguities and prompts the coder or physician to close documentation gaps instantly.
Seamless Integration
Secure APIs push coded data directly to your EHR or billing system—no re-entry needed.
Smart Feedback
Optional feedback reports help providers improve documentation over time.
This AI medical coding platform adapts seamlessly to any workflow. Use it for fully automated coding or to support your coding team.
MedGenX features a built-in AI Coding Assistant that serves as your coder’s co-pilot—smart, fast, and always compliant.
Use Cases / Specialties
Ensure smarter coding—across all specialties.
Cardiology
Chiropractic
Family Medicine
Gastroenterology
Inpatient
Neurology
Neurosurgery
Orthopedics
Outpatient
Pain Management
Pathology
Physical Therapy
Radiology
Surgery
Vascular Surgery
Why Choose MedGenX?
Built by coders for coders, MedGenX drives measurable results:
Benefit
What It Means for You
Faster Claims Processing
Complete coding in 30 seconds/chart, speeding up revenue cycles.
99.9% Coding Accuracy
50+ Specialties
Denials Reduction
Revenue Optimization
100% Compliance
Enhanced Productivity
Cost Efficiency
Better Care Delivery
Ready to see MedGenX in action?
Manual Coding vs. MedGenX AI Coding
With AI, there’s no competition!
| Feature/Aspect | Manual Medical Coding | AI-Powered Coding (MedGenX) |
|---|---|---|
| Speed | Hours per chart | 30 seconds to 3 minutes per chart |
| Accuracy | Prone to human error | 99%+ accuracy with AI + coder review |
| Compliance | Relies on coder’s knowledge | Automated updates to latest standards |
| Audit Readiness | Manual checks, time-consuming | Built-in audit trail, instant review |
| Scalability | Limited by team size | Scales instantly, no extra hiring |
| Cost | High labor costs | Lower operational costs |
| Revenue Optimization | May miss coding opportunities | Detects missed codes, boosts revenue |
| Integration | Manual data entry, risk of errors | Seamless EHR/RCM integration |
| Learning & Improvement | Slow, requires retraining | Continuous learning from feedback |
| Handling Complexity | Challenging for high-volume/specialty | Handles all specialties, batch coding |
| Error Detection | Manual review, may miss errors | Automated error flagging |
| Documentation Gaps | May overlook missing info | Prompts for missing documentation |
| Security | Process dependent | HIPAA-compliant, encrypted |
Manual Review
- Speed:Hours per chart
- Accuracy:Prone to human error
- Compliance:Relies on coder’s knowledge
- Audit Readiness:Manual checks, time-consuming
- Scalability:Limited by team size
- Cost:High labor costs
- Revenue Optimization:May miss coding opportunities
- Integration:Manual data entry, risk of errors
- Learning & Improvement:Slow, requires retraining
- Handling Complexity:Challenging for high-volume/specialty
- Error Detection:Manual review, may miss errors
- Documentation Gaps:May overlook missing info
- Security:Process dependent
AI-Powered Review
- Speed:30 seconds to 3 minutes per chart
- Accuracy:99%+ accuracy with AI + coder review
- Compliance:Automated updates to latest standards
- Audit Readiness:Built-in audit trail, instant review
- Scalability:Scales instantly, no extra hiring
- Cost:Lower operational costs
- Revenue Optimization:Detects missed codes, boosts revenue
- Integration:Seamless EHR/RCM integration
- Learning & Improvement:Continuous learning from feedback
- Handling Complexity:Handles all specialties, batch coding
- Error Detection:Automated error flagging
- Documentation Gaps:Prompts for missing documentation
- Security:HIPAA-compliant, encrypted
Talk to an Expert – Learn how MedGenX Protect your Revenue and Reduces Denials
FAQs
What is MedGenX?
MedGenX is an AI-powered medical coding platform.
How accurate is the AI medical coding process?
Our platform delivers 99% accuracy.
What sets MedgenX apart?
Can MedGenX integrate with my EHR or billing system?
Yes. MedGenX connects seamlessly through secure APIs and supports integration with all major EHRs and RCM systems. This ensures coded data flows directly into your existing workflows without manual re-entry.
Is MedGenX customizable for different workflows?
Does MedGenX only perform medical coding, or does it offer additional support?
How does MedGenX improve coder productivity?
Instead of replacing human coders, AI supports them by handling repetitive work, flagging discrepancies, and providing coding suggestions. This enables coding teams to focus on complex cases, improve overall efficiency, and reduce burnout – ultimately leading to faster turnaround times, fewer errors, and improved revenue cycle performance.
How does MedGenX reduce operational costs?
What makes OSI different from other billing services?
We have built comprehensive compliance and HIPAA programs tailored to fit the unique needs of individual practices. Our team of trained billing professionals has a proven track record of helping clients enhance profitability while easing the challenges associated with managing a billing department.
We eliminate the challenges and costs of maintaining an in-house billing department by offering a fully managed, transparent solution – complete with a flexible pricing structure and no hidden fees. With a deep understanding of your goals and a track record of delivering results, OSI ensures accurate billing, compliant claims, and timely accounts receivable recovery.
What services are available at OSI?
We understand that each provider faces unique challenges and has distinct goals, which is why we offer flexible services tailored to your needs. Our primary focus is to deliver solutions that support the long-term success of your practice. Our standard offerings include medical billing and coding, verifications and authorizations, virtual office staffing, and credentialing.



