Soft-tissue injuries (STI) are one of the most common injuries that happen due to sport and exercise activities. Sometimes simple everyday activities can also cause these injuries. The most common soft tissues injured are the muscles, tendons, and ligaments that connect, support or surround other structures and organs of the body. However, early diagnosis and appropriate treatment are essential to get better outcomes, or else soft tissue injuries can result in pain, swelling and loss of function. Proper documentation is important to ensure appropriate care and for accurate clinical documentation of STI, physicians rely on the services of reliable medical billing companies.
Soft tissue injuries are commonly categorized into two types:
- Acute injuries: Any type of injury caused by a sudden trauma, such as a fall, twists, or blow to the body. Examples of acute injury include sprains, strains, and contusions.
- Overuse injuries: An overuse injury occurs gradually over time, that is, when a certain activity is repeated frequently, and areas of the body do not have enough time to heal between occurrences. Examples include bursitis and tendinitis.
When soft tissue is damaged, there is usually immediate pain along with immediate or delayed swelling. Stiffness and bruising may also develop after 24-48 hours which is also very common as a result of the trauma and swelling. However, in the case of moderate to severe soft tissue injuries of muscles, tendons and ligaments around a joint, there may be instability experienced, especially to weight-bearing joints like the hip, knee and ankle.
Treatments for Soft-tissue Injuries
According to OrthoInfo by the American Academy of Orthopedic Surgeons, acute soft-tissue injuries vary in type and severity. When an acute injury occurs, initial treatment with the RICE (Rest, Ice, Compression, and Elevation) protocol is usually very effective. That is,
- Rest: To take a break from the activity that caused the injury in order to give the injury time to heal. Your doctor may recommend that you use crutches to avoid putting weight on your leg.
- Ice: The injured area should be cold compressed using cold packs for 20 minutes at a time, several times a day. However, avoid direct contact of the ice with the skin.
- Compression: To prevent any further bleeding or swelling from occurring, wear an elastic compression bandage to the injured area.
- Elevation: Elevate the injured part higher than your heart while resting, to reduce swelling.
However, you can also use No HARM Protocol: (Heat, Alcohol, Re-injury, and Massage), but this method should not be used within the first 48–72 hours after the injury in order to speed up the recovery process (https://en.wikipedia.org).
- Heat: Don’t apply heat to the injured area as it can increase blood flow and swelling.
- Alcohol: Alcohol can hinder the ability to feel if the injury is becoming more aggravated, as well as increasing blood flow and swelling.
- Re-injury: Avoid any activities that could worsen the injury and cause further damage.
- Massage: Even though massaging the injured area can promote blood flow and swelling, if done too early it can cause more damage.
However, if severe pain persists after the first 24hours it is recommended that the patient consult an orthopedic professional who can make a diagnosis and implement a treatment plan so the patient can return to everyday activities. To make a full diagnosis, a professional may use nerve conduction studies to localize nerve dysfunction (e.g. carpal tunnel syndrome), assess severity and help with prognosis. Electrodiagnosis also helps differentiate between myopathy and neuropathy.
Orthopedics medical billing can be challenging as it involves using several code categories. Physicians and other orthopedic specialists who perform treatments for different soft-tissue injuries must use the relevant medical codes to bill for the procedure.
Both athletes and non-athletes share many similar soft-tissue injuries. The ICD-10 medical codes used to report different soft-tissue injuries include:
-
- M70: Soft tissue disorders related to use, overuse and pressure
- M70.8: Other soft tissue disorders related to use, overuse and pressure
- M70.80 …… of unspecified site
- M70.9: Unspecified soft tissue disorder related to use, overuse and pressure
-
- M70.90: …… of unspecified site
- M70.8: Other soft tissue disorders related to use, overuse and pressure
- M79.9: Soft tissue disorder, unspecified
- Six different STI conditions and their ICD-10 codes, that affect our body’s musculoskeletal system, which require clinical care by a physician or other healthcare professional are:
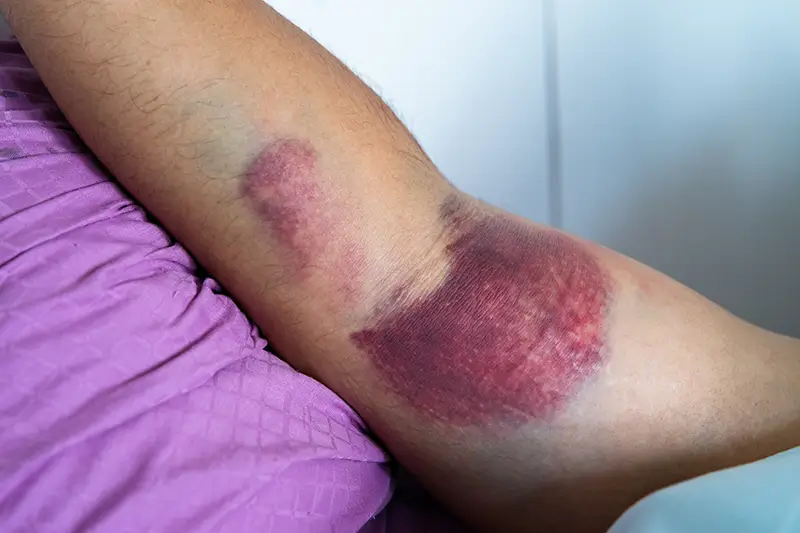
- Contusions (bruises): An injury that occurs to the soft tissue by a blunt force, such as a kick, fall, or blow. The result will be pain, swelling, and discoloration because of bleeding into the tissue. The codes are:
-
- T14.8: Contusion (skin surface intact)
- Bone NEC T14.8
- Skin NEC T14.8
- Subcutaneous NEC T14.8
- Subperiosteal NEC T14.8
- T14.8: Contusion (skin surface intact)
- Sprains: A partial tear to a ligament which is often caused by a wrench or twist. The areas of your body that are most vulnerable to sprains are your ankles, knees, or wrists. If your sprain is severe, that is, if the ligament is completely torn, then surgical repair may be necessary.
-
- S73.1: Sprain of hip
- S53.4: Sprain of elbow
- S93.4: Sprain of ankle
- S93.6: Sprain of foot
- Strains: An injury to a muscle and/or tendon caused due to overuse, force, or stretching. It often occurs in your foot, leg (typically the hamstring) or back. General symptoms of a strain include pain, muscle spasm, muscle weakness, swelling, inflammation, and cramping.
- S76.01: Strain of muscle, fascia and tendon of hip
- S76.11: Strain of quadriceps muscle, fascia and tendon
- S76.21: Strain of adductor muscle, fascia and tendon of thigh
- S76.81: Strain of other specified muscles, fascia and tendons at thigh level
- Tendonitis: A type of overuse injury to the tendons, a flexible band of tissue that connects muscle to bones. Areas commonly affected include the elbow, hand, wrist, shoulder, hip, knee, ankle, and foot. Tendonitis often named for the sport or movement that triggers the inflammation, such as tennis or golfer’s elbow, swimmer’s shoulder, and jumper’s knee.
- M75.20: Bicipital tendinitis, unspecified shoulder
- M75.30: Calcific tendinitis of unspecified shoulder
- M76.00: Gluteal tendinitis, unspecified hip
- M76.50: Patellar tendinitis, unspecified knee
- M76.70: Peroneal tendinitis, unspecified leg
- Bursitis: Caused due to inflammation of the bursa, a fluid-filled sac that provides a cushion between bones and muscles or tendons. It can also be caused due to direct trauma to a joint. Body areas such as the shoulder, elbow, knee, hip, ankle, and foot are commonly affected by this condition.
- M70: Soft tissue disorders related to use, overuse and pressure
-
-
- M71.9: Bursitis
- Stress injuries: Injuries most often caused by overuse and increase in physical activity. The most common stress fracture is a small crack in a bone, commonly occurring in the weight-bearing bones of the lower extremities, including legs, hips, and feet. If the crack in the bone progresses further to a complete break, surgery may be required.
- M84.3: Stress fracture
- M84.30: Stress fracture, unspecified site
- M84.31: Stress fracture, shoulder
- M84.34: Stress fracture, hand and fingers
- M84.37: Stress fracture, ankle, foot and toes
- M84.3: Stress fracture
-
Soft-tissue injury coding in an orthopedic practice is usually a high volume service. Medical billing companies with experience in providing documentation for this specialty can assist physicians with efficient services.