Timely filing limits play a crucial role in the healthcare revenue cycle, directly impacting whether claims are accepted or denied. Each payer sets specific deadlines for claim submission, and failure to meet these timelines can result in lost reimbursement opportunities. For healthcare providers managing multiple payers, keeping track of these varying requirements can be a significant administrative challenge.
Government and commercial insurers follow different filing rules, with deadlines ranging from a few months to a full year from the date of service. In addition, variations based on state regulations, plan types, and authorization requirements add another layer of complexity. Without a clear understanding of these timelines, providers risk claim denials, delays, and disruptions to cash flow.
In such scenarios, partnering with an experienced medical billing company can reduce administrative burden and improve submission accuracy. Skilled billing professionals stay updated on payer-specific requirements, ensuring that claims are filed within stipulated timelines and in compliance with current regulations. This level of external support not only minimizes the risk of denials due to missed deadlines but also contributes to a more consistent and efficient revenue cycle management process.
The infographic below highlights key deadlines and important considerations, helping providers improve claim accuracy and maintain a more efficient medical billing workflow.
Check Out the Infographic
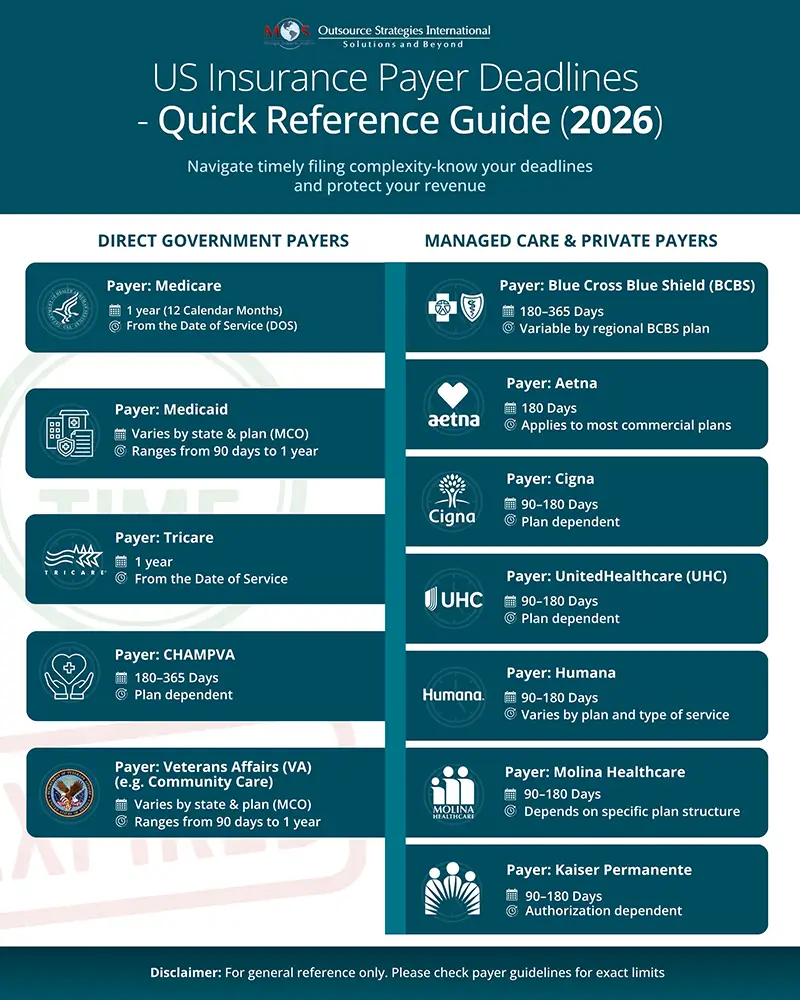
Don’t let rigid payer deadlines dictate your cash flow.




