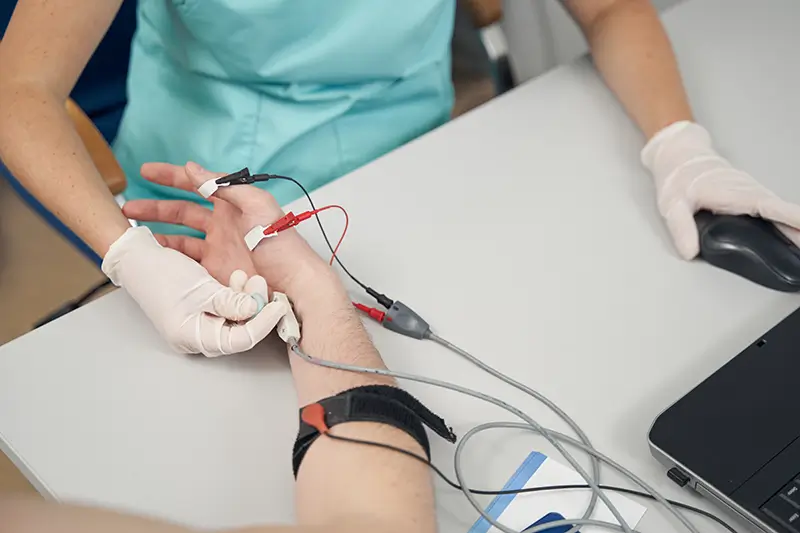
Nerve conduction studies (NCS) measure how fast electrical impulses travel along the nerves. A nerve conduction test is usually performed in conjunction with electromyography (EMG) which evaluates the electrical functioning of muscles. These electrodiagnostic (EDX) tests are used to help in the diagnosis of a variety of nerve and muscle disorders. Neurology medical billing and coding can be complex as there are specific codes for every diagnostic service and treatment. Up-to-date professional billing and coding guidance can be crucial for the submission of claims for reimbursement of covered services.
Here are 4 key tips to help with nerve conduction study coding:
1.Select the correct code based on the number of nerves tested: Choosing the correct code depends on the number of nerve conduction studies performed. The CPT codes for NCS are:
- 95905 Motor and/or sensory nerve conduction, using preconfigured electrode array(s), amplitude and latency/velocity study, each limb, includes F-wave study when performed, with interpretation and report
- 95907 1-2 nerves
- 95908 3-4 nerves
- 95909 5-6 nerves
- 95910 7-8 nerves
- 95911 9-10 nerves
- 95912 11-12 nerves
- 95913 13 or more nerves
CPT defines a single conduction study is: “a sensory conduction test, a motor conduction test with or without an F wave test, or an H-reflex test.” CPT lists individual nerves for billing NCS. The list identifies each individual sensory, motor, or mixed nerve, or nerve segment that can be counted separately toward the NCS total. Each list of nerves refers to a different nerve and should be counted as an individual unit. For e.g., the 4 different nerve segments of the ulnar motor nerve can each be counted separately toward the total.
– Each type of study is counted as a distinct study.
– If the provider performs stimulation or recording of multiple sites on a single nerve during a single study, this should be still counted as a single study. For e.g., testing the ulnar nerve at wrist, forearm, below elbow, above elbow, axilla and supraclavicular regions are all considered as a single nerve.
– Multiple NCS CPT codes cannot be billed for a given patient on a single day
The American Association of Neuromuscular & Electrodiagnostic Medicine (AANEM) recommends that physicians test the fewest number of nerves needed to assess or diagnose a medical issue when performing an NCS. The physician should provide supplementary documentation to justify any additional testing and its medical necessity.
2.Report EMG when performed: Electrodiagnostic tests (EDX) cover a range of specialized tests, including nerve conduction studies (NCS) and needle electromyography (EMG).Individual tests should be reported using the NCS code as the primary code and EMG codes as add-on codes. The add-on codes for the EMG are:
- 95885 Needle electromyography, each extremity, with related paraspinal areas, when performed, done with nerve conduction, amplitude and latency/velocity study; limited (List separately in addition to code for primary procedure)
- 95886 Needle electromyography, each extremity, with related paraspinal areas, when performed, done with nerve conduction, amplitude and latency/velocity study; complete, five or more muscles studied, innervated by three or more nerves or four or more spinal levels (List separately in addition to code for primary procedure)
- 95887 Needle electromyography, non-extremity (cranial nerve supplied or axial) muscle(s) done with nerve conduction, amplitude and latency/velocity study (List separately in addition to code for primary procedure). Checking payer policies in important to know which neurology diagnoses support coverage for testing.
3.Adhere to payer guidelines: To bill and code nerve conduction studies correctly, providers need to be aware of the latest codes as well as the reimbursement policies of governmental and private payers. For instance, the Centers for Medicare & Medicaid Service (CMS) guidelines on CPT code 95905 are as follows:
-
- Nerve conduction studies done using preconfigured electrode array(s) using automated devices, such as NC- stat® System, cannot support testing of other locations and other nerves as needed depending on the concurrent results of testing and must not be billed with any CPT code other than 95905.
- When the beneficiary has a high pre-test or a priori probability for a Carpal Tunnel Syndrome diagnosis, the automated devices alone will be allowed, one service per arm, using code 95905 along with diagnosis codes G56.00-G56.03 only.
- Code 95905 is payable only once per limb studied and cannot be used in conjunction with any other nerve conduction codes.
- Code 95905 is not allowed to be billed by physical therapists.
4. Document medical necessity: To avoid having claims denied, providers should report diagnoses to inform the payer why a service was performed and support medical necessity of the nerve conduction study and needle electromyography. Every CPT code should be paired with an ICD code that demonstrates the medical necessity. Government and commercial health insurance payers state the criteria that nerve conduction studies and needle electromyography need to meet to be considered medically necessary, and which procedures are considered unproven and medically unnecessary. AANEM clarifies:
-
- Nerve Conduction Studies EDX testing with automated, noninvasive nerve conduction testing devices is considered investigational and not medically necessary for all indications.
- Screening testing for polyneuropathy of diabetes or end stage renal disease (ESRD) is NOT covered. Testing for the sole purpose of monitoring disease intensity or treatment efficacy in these two conditions is not covered.
- Psychophysical measurements (electrical, vibratory or thermal perceptions) are not covered. Current Perception Threshold/Sensory Nerve Conduction Threshold Test (sNCT) is investigational and not covered.
The patient’s health plan and the regulations laid out by the payer determine whether a procedure is billable. Reliable neurology medical billing company have teams of expert coders and billing specialists. Coders will report the correct diagnostic code for each diagnostic test ordered and the billing team will review the codes reported to ensure that the procedures coded are billable. With their knowledge of the latest codes and coverage policies of each payer, neurology medical billing for nerve conduction tests can help practitioners avoid claim denials.