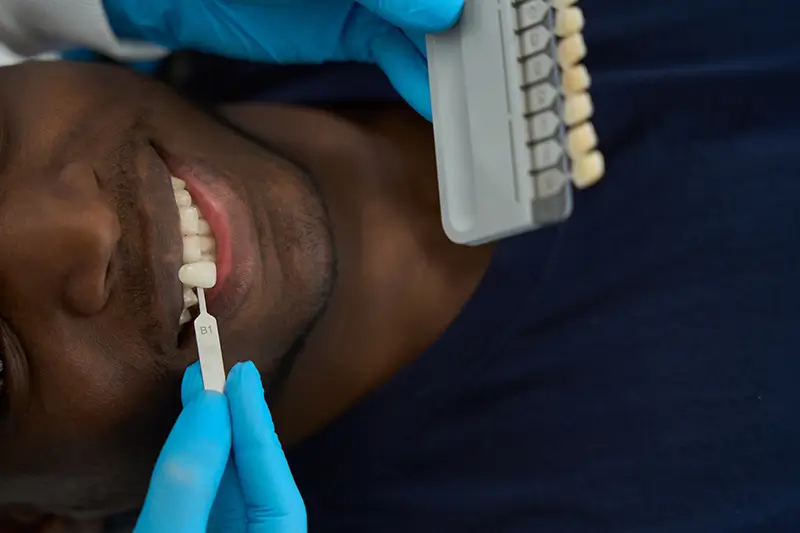
Dental insurance plans provide coverage for certain dental procedures. According to the National Association of Dental Plans, up to 77% of Americans have dental benefits. Some plans cover a percentage of the cost of basic services, while others pay for some of the cost of both basic and major work. Dental benefits are complex, differ among plans and by insurance company, and may change yearly. Many dental plans also have exclusions such as the missing tooth clause. Dentists can work with their dental billing company to help patients understand the details of their coverage and make the most of it.
Understanding the Missing Tooth Clause
Similar to medical insurance, a dental plan may not cover a condition a person had before enrolling in the plan. The missing tooth clause in dental insurance is similar to this pre-existing condition exclusion in medical insurance, but more specific. More than 50% of dental plans have this clause.
Both patients and their provider need to understand the policies, terms, and conditions of the missing tooth clause. The reason why this clause confuses the dental team is that the insurance plan may state that the prosthesis is covered at 50%, with the patient paying the balance.
A missing tooth clause is a contractual provision in a dental insurance plan whereby the insurance company candeny coverage for the cost of the tooth replacement procedure if the tooth was lost, extracted or removed before the patient’s coverage takes effect. This clause may also apply to a congenitally missing tooth. In this situation, the patient will pay entirely out of pocket for the tooth replacement, whether it is a bridge, crown, fixed partial denture, removable partial, or implant. This can be expensive.
Another thing to look for in a dental policy is the waiting period. Key points:
- In some cases, the insurance policy will cover tooth replacement costs after a waiting period is over.
- If the missing tooth clause includes a waiting period, the plan will not cover a tooth replacement if the tooth was lost during this waiting period.
- Waiting periods vary among insurance company and usually range from a few months to one year. However, some policies have waiting periods that extend to five years.
Not all dental policies have a missing tooth clause. For instance, Delta Dental does not have a Missing Tooth Exclusion. Delta Dental covers the tooth replacement procedures for members who had a tooth fall out or extracted prior to having dental coverage with Delta Dental.
Certain Cigna PPO plans have a Missing Tooth Clause. Cigna states:”If a bridge replaces teeth that were missing prior to the date the person’s coverage became effective and also teeth that are extracted after the person’s effective date, benefits are payable only for the pontics replacing those teeth which are extracted while the person was insured under this plan’.
Patients should be advised to read the fine print of their dental plans and be aware about what is covered and what is not, including the missing tooth clause. If the insurance policy has a missing tooth clause and the patient still want the treatments, a predetermination can be set up.
How Predeterminations can Help
Some plans recommend obtaining predeterminations for procedures exceeding a specific dollar amount. Such procedures include extractions, crowns, onlays, veneers, fixed bridgework, implants or periodontal treatments.
The American Dental Association defines a predetermination as “an estimate of who pays what for the service’. Predeterminations or pretreatment estimates of patient eligibility for coverage are a useful strategy for dental offices when working with patients to obtain their consent for desired treatment plans. It will help them understand what they have to pay out of pocket after any coinsurance, deductible, and policy maximum. With a predetermination, patients will have the information required to make an informed financial decision about their treatment.
Once the diagnosis in complete, you should provide the patient with a treatment plan, which will help them determine how to pay for their treatment. The insurance company can be asked to review that treatment plan. Your office can send an appeal along with the proper documentation to overturn the original decision. According to www.stgeorgesmiles.com, insurance companies may waive the missing tooth cause if the tooth was extracted within 3 years of the proposed replacement date.
Dental Insurance Verification Services to Understand Patient Coverage
If patients do not understand or miss reading or a missing tooth clause, they may end up paying much more than expected. Dental verification, which is first step in dental billing, can resolve this challenge. Dental insurance verification services provided by dental billing companies can help your front office clearly understand details of patient coverage before treatment is provided. This includes details on the type of plan, coverage, payable benefits, plan exclusions such as the missing tooth clause, and much more. With the reports provided by your dental billing company, you can educate patients about the specific details of the insurance plan and help them make informed decisions, which will build their trust in your dental practice. It will also ensure proper billing to avoid loss in insurance payments.