Years of Experience
Happy Clients
Experienced Professionals
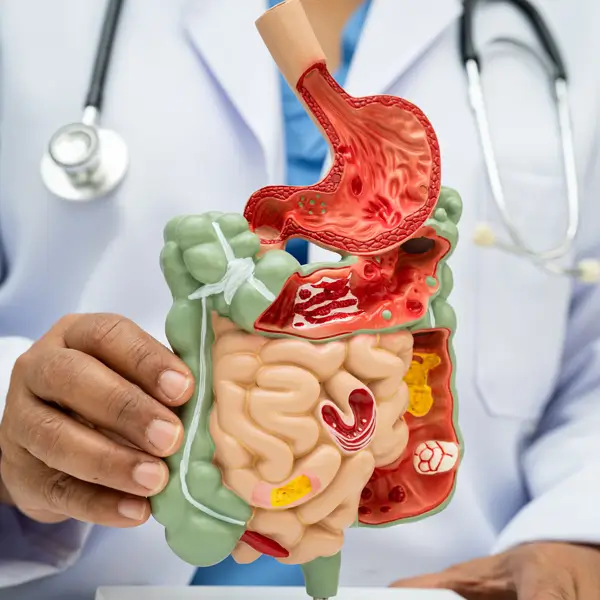
Simplify Gastroenterology Medical Billing, Maximize Revenue
We can provide custom solutions to optimize your claim submission and reimbursement as you focus on patient care. Our GI medical billing company is well-equipped to handle all the complexities associated with the claim submission process. Our certified coders have gastroenterology-specific coding skills and our billing specialists will ensure clean claims for accurate reimbursement.
End-to-End Gastroenterology Medical Billing Services
We will work as an extension of your practice to deliver the following services:
Insurance Verification
Real-time verification of coverage, plan details, benefits, and deductibles. This reduces risk of claim denials and streamlines billing.
Read More
Prior Authorization
Read More
Charge Capture
Documenting all billable services to ensure accurate coding and invoicing. This is crucial for timely and appropriate payment for services.
Read More
Coding
Read More
AR Management
Read More
Reporting and Analysis
Creating customizable reports to provide insights into your practice’s financial performance. This allows you to make more informed decisions.
Read More
Key Gastroenterology Billing Codes
Gastroenterology practices perform many diagnostic and therapeutic procedures. We understand the procedural complexity and coding challenges in gastroenterology billing. Our billers are experienced in high volume services such as:
- 45378 – Colonoscopy (diagnostic)
- 45380 – Colonoscopy with biopsy
- 45385, 45384 – Colonoscopy with polypectomy
- 43235 – Upper Endoscopy (EGD)
- 43239 – EGD with biopsy
- 45330 – Flexible sigmoidoscopy
- 43248 – Esophageal dilation
Our team maintains accuracy across the entire billing cycle to ensure complete reimbursement and compliance with regulations. For many practices, choosing to outsource GI billing not only helps control costs but also enhances claims turnaround times and overall revenue performance.
Modifier Usage in GI Billing
Modifiers are crucial in GI billing as they convey the procedure details to the payers. Correct application can make the difference between full payment and claim denial.
- Modifier 33 – For preventive services under the ACA (e.g. screening colonoscopy).
- Modifier PT – When a screening colonoscopy is converted to diagnostic due to a finding (e.g. polyp removal).
- Modifier 59 – Shows that a procedure is performed separately, distinct from the one usually reported together.
- Modifier 51 – When multiple procedures are performed during the same session.
We make sure that the claims are submitted with proper modifiers so your practice does not lose payments that it rightfully deserves.
Bundled Procedures and Denial Trends
Incorrect modifier usage or not following the bundling rules can lead to common denial scenarios.
Common Denial Trends:
- Modifier and Coding Errors – Misuse of modifiers, such as using PT to a diagnostic colonoscopy, is a leading reason for denial.
- Unbundling Errors – Services that should be bundled, like multiple biopsy sites during a colonoscopy, may be denied if reported separately.
- Lack of Prior Authorization – Some procedures, like advanced diagnostic tests, require payer pre-approval.
- Incomplete Documentation – If the medical records do not reflect adequate detail to justify the procedure, payers may deny the claim.
As a trusted provider of gastroenterology RCM services, we minimize these denials through:
- Real-time claim scrubbing for modifier accuracy
- Pre-submission audits to ensure documentation and coding compliance
- NCCI-compliant practices
- Denial tracking, trend analysis, and proactive appeals management
By staying ahead of these issues, we provide faster reimbursement and less administrative hassle.
Why Choose OSI?
Here’s why we’re the ideal choice to be your medical coding partner:
- AAPC-certified coders with expertise in gastroenterology coding
- Experts that stay current with the latest coding guidelines from AMA and CMS
- Robust quality assurance process to minimize errors
- Claim submission to meet payer and industry regulations
- Use of advanced coding software to enhances the speed and accuracy of coding
- Seamless integration with your practice’s EHR system
- Real-time reports and analytics to monitor practice performance
- Strong data security measures to protect sensitive patient information
We serve all 50 states
Highlights of Our Services
- Dedicated manager
- HIPAA compliance
- Regular QA checks
- Customized TAT
- No long-term yearly contracts
- No initial costs or hidden fees
- Savings of 30% to 40%
- Daily, monthly and weekly reports
Gastroenterology Medical Billing and Coding Process
Here’s an overview of our medical billing process:
1
Patient Registration
1
Patient Registration
Our Pricing Plans
Full-Time Equivalent
At present, we provide only the FTE pricing model for Accounts Receivable (AR). We are also considering a blended model for AR.
FAQs
Do you follow up on unpaid claims?
Yes, we do.
Our billing experts thoroughly evaluate your accounts receivable position and identify denied claims, unpaid claims, and low payments. Claims are re-submitted with any additional information needed. With timely follow-up and appeals, we help accelerate your cash flow and minimize accounts receivable days.
How do you manage patient collections?
Our patient responsibility management services include sending patient statements in a timely manner (sometimes adjusted according to client preference). In addition, we follow up with a demand letter and phone calls. We see that timely follow-up helps in obtaining quicker reimbursement. If for any reason we find the efforts futile, we will work with a collection agency or an attorney for collections if our client feels that step is necessary
Is OSI HIPAA-compliant?
Yes, we are fully compliant with HIPAA rules and standards. Our stringent data security policies are designed to ensure that all patient information remains safe and secure. Security measures are taken in-house as well as during the transfer of files. Our entire workforce is trained on privacy, security, and confidentiality, and all our employees must sign a confidentiality and non-disclosure agreement. Contractual agreements with all business parties are maintained and up-to-date.
How do you work with your clients? Do we have to give you our whole revenue cycle management to start with you?
Related Posts
Why is Insurance Preauthorizations a Major Challenge for Gastroenterology Practices
by Natalie Tornese | Posted: Dec 4, 2020
ICD-10 Codes to Report Peptic Ulcer – A Common Gastrointestinal Disorder
by Julie Clements | Posted: May 19, 2023
Medical Coding for Irritable Bowel Syndrome
by Natalie Tornese | Posted: Sep 19, 2023