Years of Experience
Experienced Resources
Satisfied Clients
Streamline Your Vascular Practice with Expert Billing and Coding Services
Navigating complex vascular medical billing and coding can be a daunting task. With ever-changing regulations and intricate coding systems, it’s easy to fall behind and lose valuable revenue.
Maximize Revenue with Superior Vascular RCM Services
Insurance Verification
Read More
Prior Authorization
Read More
Charge Capture
Capturing the full value of every procedure performed to ensure accurate coding and invoicing This is crucial for correct coding to maximize financial performance
Read More
Precise Coding
Read More
AR Management
Read More
Reporting and Analysis
Read More
Why Choose Our Vascular Medical Billing Company

- Dedicated manager on your project
- HIPAA compliance
- Regular QA checks
- Customized TAT
- No long-term yearly contracts
- No initial costs or hidden fees
- Savings of 30% to 40%
- Daily, monthly and weekly reports
Leverage Vascular Coding Expertise
Variation in presentation, pathology, and procedure strategy
Inherent anatomical complexity
Frequent changes to coding structure
- AAPC-certified coders specialized in ICD-10, CPT and HCPCS coding
- Experts updated on AMA and CMS coding guidelines
- Strong quality assurance to minimize errors
- Compliance with payer and industry regulations
- Advanced software for faster, accurate coding
- Seamless integration with your EHR system
- Real-time reports to track practice performance
- Robust data security for patient information protection
We serve all 50 states
Our Medical Billing and Coding Process
1
Patient Information Collection
Coding
Follow-Up
1
Patient Information Collection
Flexible Pricing Options
Full-Time Equivalent
At present, we provide only the FTE pricing model for Accounts Receivable (AR). We are also considering a blended model for AR.
FAQs
How do you ensure coding accuracy?
Can you integrate your services with our EHR system?
How do you handle denied or rejected claims?
What measures do you take to protect patient data?
How often do you provide reports on billing performance?
What is the turnaround time for claim submission?
Can you help with patient billing and collections?
What support is available if I have questions or issues?
Related Posts
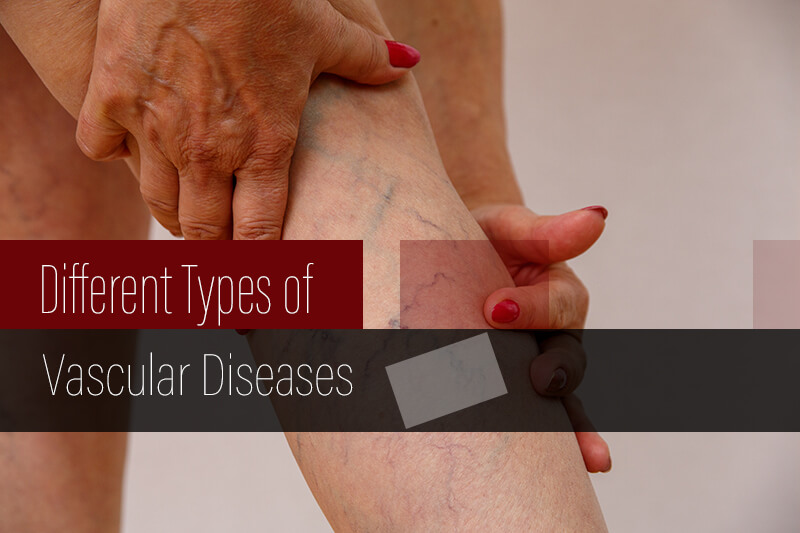
Coding Different Types of Vascular Disease – A Look at the Related ICD-10 Codes
Medical Codes to Report Vascular Dementia
Medical Coding for Lymphedema – A Common Vascular Disease
by Julie Clements | Posted: Nov 22, 2022