Automation has revolutionized almost every facet of life and work. The medical billing process is also undergoing a transformation with the integration of AI applications, resulting in increased speed, enhanced accuracy, and reduced risk of errors. However, despite these advancements, it is crucial not to overlook the indispensable role of human expertise in providing medical billing services.
“While the EMR/EHR automate the claims, we still have to review them before they are sent out. The automation is always missing critical things like modifiers that can be used to get the claim paid”, says Natalie Tornese, OSI’s AAPC CPC, Director of Revenue Cycle Management – Healthcare Division.
Let’s dive into why human involvement in the medical billing process is so crucial.


Optimize your financial workflow with medical billing services tailored to your needs!
Why Human Involvement in Billing Matters
Here are the key reasons why human experts are still essential in medical billing:
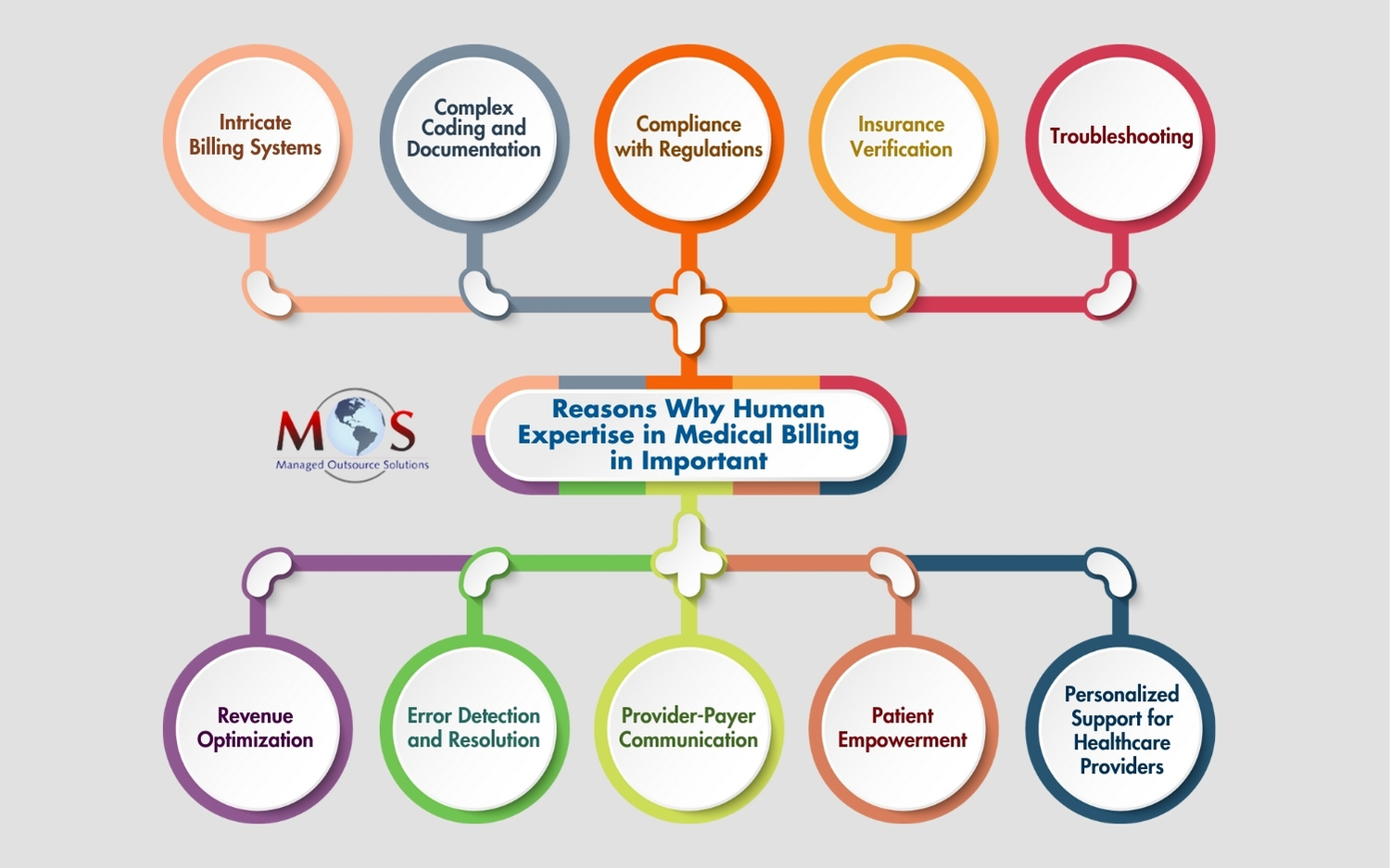
Intricate Billing Systems
A billing system is a complex software with various components such as pricing structures, discounts, and contractual agreements. It generates and automates processes such as payments, invoices, revenue management, and various other functionalities. However, lack of proper oversight increases the risk of errors within the system, potentially resulting in claim denials. This not only impacts the financial stability of the healthcare provider but also hinders the patient’s access to healthcare services.
Human expertise is crucial for understanding and interpreting these complexities accurately. Trained professionals are needed to analyze recurring revenues, business data, and generate detailed reports, and perform in-depth analytics. Resolving intricate medical billing issues frequently requires human intelligence and judgment. In specific or uncommon situations, artificial intelligence may prove inadequate.
Complex Coding and Documentation
Medical billing involves translating complex medical procedures, diagnoses, and treatments into specific codes for accurate billing and reimbursement. Human billing and coding experts have in-depth knowledge of coding systems such as Current Procedural Terminology (CPT) and International Classification of Diseases (ICD) as well as modifier use. They can accurately assign the appropriate codes based on the medical documentation, ensuring compliance and maximizing reimbursement.
Compliance with Regulations
Billing in the healthcare industry is subject to numerous regulations and guidelines, such as those set by government payers (e.g., Medicare, Medicaid) and private insurance companies. Human billing experts know how to navigate the intricate landscape of different payer policies, always-changing coding updates, and changing regulations. They stay informed about these changes and adapt billing practices accordingly. They can navigate updates to coding systems, documentation requirements, and reimbursement methodologies.
Their expertise is crucial to ensure healthcare providers get proper reimbursement for their services. By ensuring medical coding compliance and accurate billing, they see that healthcare providers don’t get hit with penalties, audits, or legal issues.
Insurance Verification Process
Automated systems are designed to verify patient eligibility in real time. However, when it comes to communicating with insurance companies to resolve any discrepancies or obtain additional information, human expertise is crucial. Consider a patient scheduled for a medical procedure that requires pre-authorization from their insurance provider. The automated patient eligibility verification system may check basic information such as the patient’s coverage status and deductible amount. However, it may overlook specific details or changes in the insurance policy that could affect coverage for the procedure.
In contrast, a human insurance verification specialist would have the ability to thoroughly review the patient’s insurance policy, including any recent updates or changes. They could identify nuances in the policy that an automated system might miss, such as specific exclusions or limitations related to the procedure in question. They will communicate with the payer, ask targeted questions, and provide necessary documentation to ensure accurate verification of coverage. Additionally, human specialists possess experience and expertise in navigating complex insurance policies and guidelines. They can interpret and apply insurance rules and regulations more effectively, ensuring accurate verification and minimizing the risk of claim denials or delays.
Troubleshooting
Although AI and automation can identify issues, they might lack the creative problem-solving abilities required to address specific billing challenges. “Sometimes you have to get really creative to get a claim paid”, notes OSI’s billing and coding expert. “A billing expert knows how to get ahead of “by the book” claims and denials,” she says.
Revenue Optimization
Billing experts understand the complexities of insurance contracts, reimbursement rates, and billing regulations. They utilize their expertise in coding and documentation to optimize revenue for healthcare providers and reduce the risk of claim denials or underpayments.
Error Detection and Resolution
Human billing experts are skilled at identifying errors or discrepancies in medical documentation, coding, and billing processes. They perform thorough reviews of claims and documentation, ensuring accuracy and identifying potential issues that could lead to claim denials or delays. They can address and resolve issues promptly, reducing the risk of revenue loss.
Provider-Payer Communication
Billing experts act as intermediaries between healthcare providers and insurance companies. They communicate with payers to resolve claim inquiries, clarify coding or documentation issues, and negotiate fair healthcare reimbursement rates. Their expertise in payer requirements and industry standards helps facilitate effective communication and promotes smooth payment processes.
Patient Empowerment
Billing experts play a vital role in helping out patients by ensuring accurate and fair billing practices accurate and fair. When it comes to answering questions, sorting out problems, and setting up payment plans, billing specialists interact with patients. They explain insurance coverage, go over billing stuff, and help sort out any billing disputes. Their know-how is key in keeping patients safe from incorrect charges, surprise bills, or unfair billing practices. Making a connection and gaining trust from patients is a vital aspect in healthcare billing, and that’s something only a personal, human touch can achieve.
Personalized Support for Healthcare Providers
Human billing experts provide personalized support to healthcare providers, addressing their specific needs and challenges. They can offer guidance on documentation improvement, coding accuracy, and revenue cycle management strategies. Additionally, they are available to address inquiries, handle claim appeals, and resolve billing-related issues through direct communication and problem-solving.
Can AI Replace Medical Billing and Coding Professionals?
While automation and technology play a role in streamlining medical billing and coding processes, these advancements cannot replace the expertise and human judgment of billing and coding professionals. Human experts bring a strategic perspective to billing processes, aligning them with broader business objectives. They can analyze billing data to identify trends, optimize pricing strategies, and contribute to revenue growth. Yet, machine learning can handle numerous routine medical billing tasks that consume resources, diverting attention from healthcare organizations striving to enhance patient services. It is likely that we can expect a hybrid approach in the foreseeable future, where AI technology and machine learning will collaborate with human expertise. This can free up staff in a medical billing and coding company from doing the mundane tasks and allow them to focus on the critical aspects of revenue cycle management.





