In medical revenue cycle management, claim denials continue to impact cash flow, operational efficiency, and administrative workload. Even a small percentage of denials can lead to significant revenue leakage and delays in insurance reimbursement. Most claim denials originate from errors in different stages of the medical billing process, and include:
- Patient eligibility issues
- Coding inaccuracies
- Missing or incomplete documentation
In many cases, recurring denials are preventable. However, repeat denials often indicate deeper issues, such as inefficient front-end workflows, improper coding practices, or weak denial follow-up systems. Understanding denial categories and associated remittance codes is essential to implement a structured RCM denial management process.
What Is RCM Denial Management?
RCM denial management involves identifying, analyzing, and resolving claim denials using remittance codes and structured workflows. By improving front-end processes, ensuring accurate coding, and leveraging AI-driven tools, healthcare providers can reduce repeat denials, improve claim acceptance rates, and accelerate insurance reimbursement.
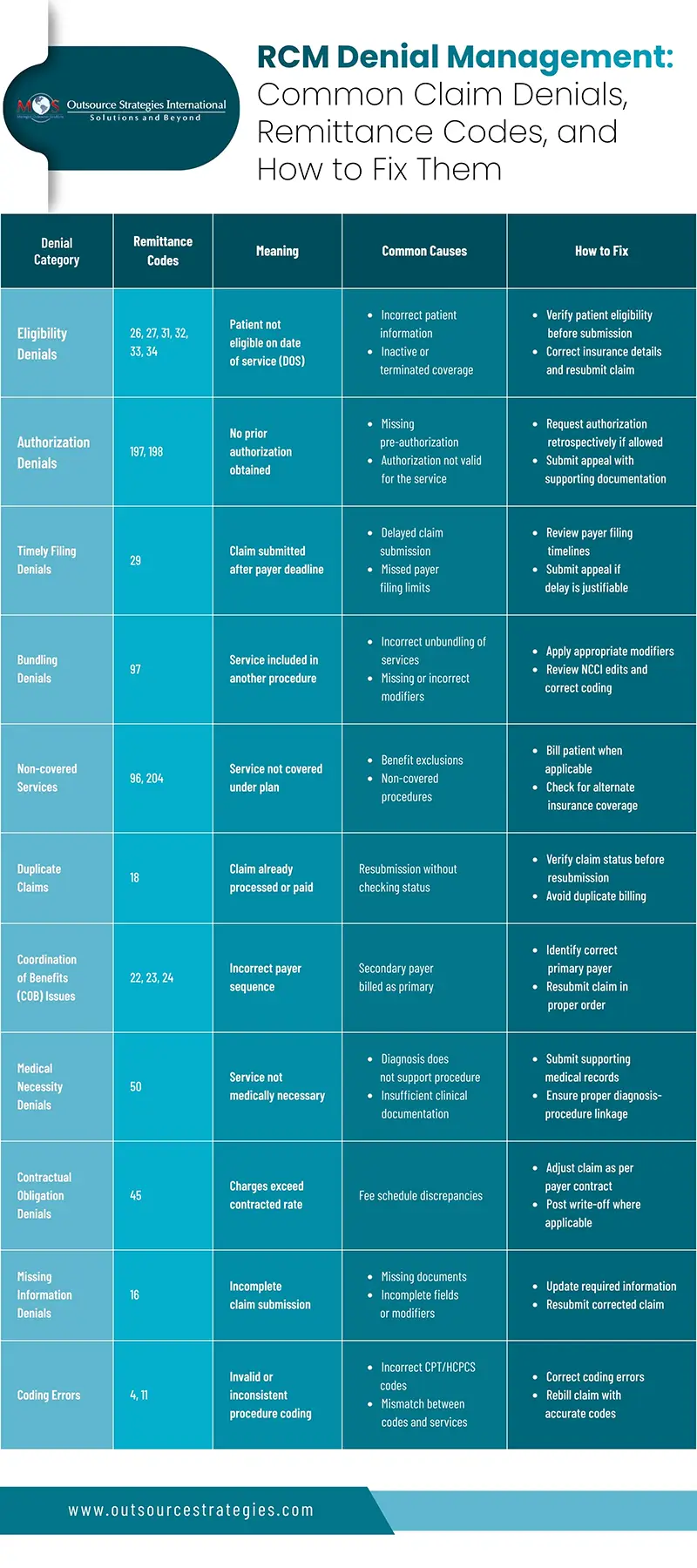
Understanding Common Medical Claim Denial Reasons and Remittance Codes in RCM
Claim denials are grouped into specific categories based on the underlying issue identified by the payer. Each denial is associated with a remittance code, which provides standardized insight into why a claim was rejected during claim adjudication.
Understanding these categories helps billing teams identify patterns, correct errors effectively, and reduce repeat denials.
Step-by-Step Denial Management Workflow in RCM
A structured workflow improves denial resolution rates and reduces AR days.
- Review EOB/ERA
Analyze Explanation of Benefits (EOB) or Electronic Remittance Advice (ERA) to identify denial codes, payment adjustments, and payer remarks.
- Identify Denial Reason and Remittance Code
Interpret remittance codes to determine the root cause—eligibility, coding, authorization, or documentation.
- Check Payer Portal for Additional Details
Use payer portals for deeper insights, including documentation requirements and claim history.
- Correct and Update Claim Information
Update patient details, coding, modifiers, or supporting documentation as needed.
- Resubmit Claim or Initiate Appeal
Resubmit corrected claims or initiate appeals with proper justification.
A consistent workflow strengthens the denial management process and reduces repeat denials.
Key Strategies to Reduce Claim Denials
Effective RCM denial management focuses on prevention, not just correction.
-
- Front-end Eligibility Verification: Real-time eligibility checks ensure accurate patient and insurance data, preventing avoidable denials.
- Accurate Coding and Modifier Usage:
Errors in ICD-10, CPT, and HCPCS coding are a major cause of denials. An AI-driven medical coding tool like MedGenX, powered by DeepKnit AI, can:
-
- Analyze clinical documentation
- Suggest accurate codes
- Flag inconsistencies in real time
- Timely Claim Submission: Automated workflows and internal benchmarks help meet payer deadlines and avoid timely filing denials.
- Strong Documentation Practices: Clear, complete documentation supports medical necessity and reduces rejection risk.
- Denial Trend Analysis: Tracking denial patterns helps identify root causes.
AI-powered analytics can improve decision-making and reduce repeat denials. - Staff Training and Process Standardization: Regular training and standardized workflows improve accuracy and consistency across the revenue cycle.
A combination of strong operational practices and technology-driven support helps reduce denial rates, improve claim accuracy, and ensure more efficient revenue cycle management.
How an RCM Partner Can Make a Difference
A well-defined denial management strategy requires both operational discipline and advanced technology.
A reliable healthcare RCM partner providing AI-powered medical RCM services can help:
- Implement structured denial follow-up systems
- Improve claim accuracy and compliance
- Leverage automation and analytics
- Reduce administrative burden
This results in:
- Faster reimbursements
- Lower denial rates
- Improved cash flow
Prevent Claim Denials with Reliable RCM Management
RCM denial management is not just about fixing rejected claims—it’s about building a system that prevents them.
By combining:
- Strong front-end processes
- Accurate coding
- Real-time eligibility checks
- AI-driven tools
Healthcare providers can significantly improve insurance reimbursement outcomes and overall revenue cycle performance.
Improve your first-pass claim rate with advanced denial prevention strategies.