While healthcare organizations focus on delivering quality care, getting paid for their services remains a challenge. Claim denials are claim denials are one of the most persistent sources of revenue leakage in healthcare. In 2025, hospitals and clinics lost over $48 billion in revenue due to denied claims and unpaid bills, a 25% increase from the previous year, according to a new study. The MGMA Stat Poll found that 60% of medical groups reported an increase in claim denials in 2024 compared to 2023.
Claim denials disrupt cash flow by withholding earned revenue, force providers to dedicate significant staff time to rework and appeals, and prolong the reimbursement cycle. Apart from the immediate financial impact, denials increase administrative workload, divert attention from patient care, and pose compliance risks. Failure to implement strong denial management strategies leads to revenue cycle inefficiencies, lower workforce productivity, and billing disputes that can affect patient trust and satisfaction.
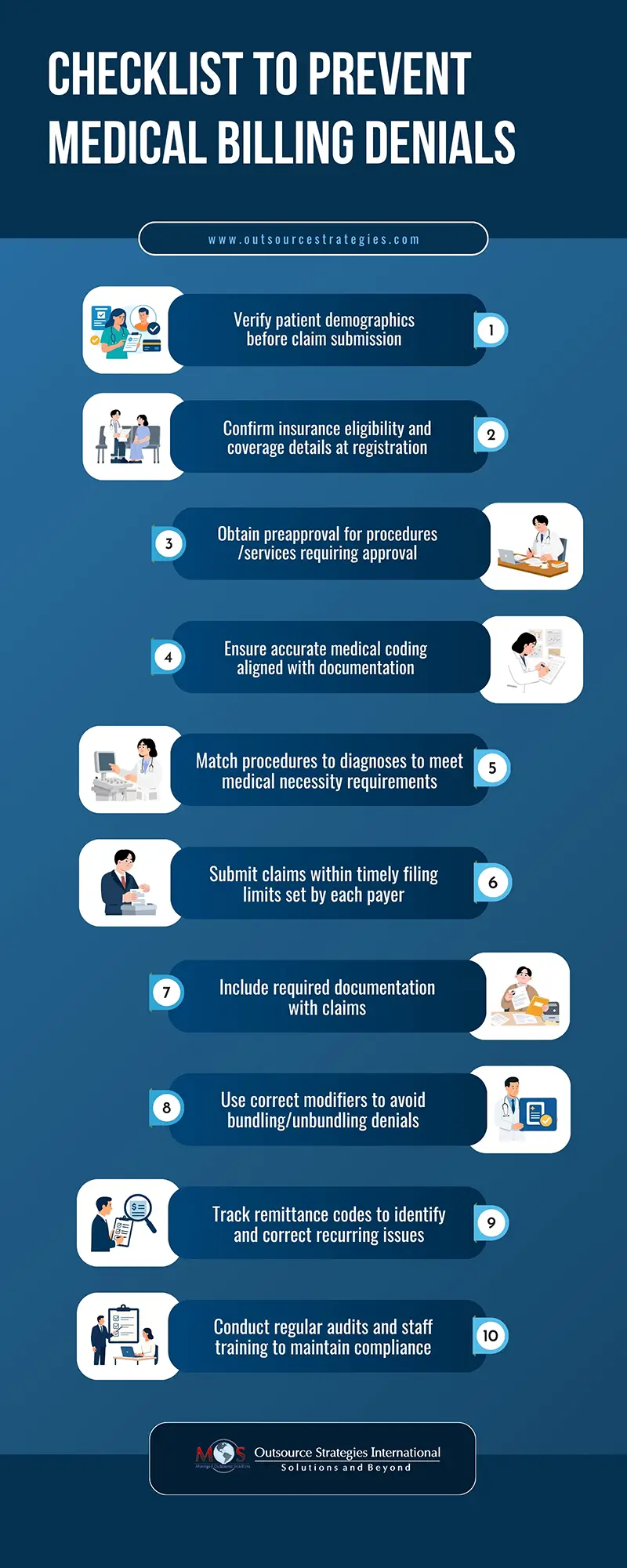
This post covers what denial management is, common reasons for claim denials, types of denials, effective solutions, and how AI and automation improve the process.
Struggling with rising denials?
Enhance your denial management process and recover lost revenue faster with our expert support.
What is Denial Management in Healthcare?
Denial management is the systematic process of identifying, analyzing, and resolving claim denials through the use of remittance codes and structured workflow. By strengthening front-end processes, ensuring precise medical coding, and adopting AI-powered tools, healthcare providers can minimize recurring denials, boost claim acceptance rates, and accelerate reimbursement from insurers. Effective strategies not only safeguard revenue but also enhance operational efficiency and reduce administrative burden.
Before we explore how to handle insurance claim rejections efficiently, it’s important to understand the different types of denials that healthcare providers face
Types of Medical Claim Denials
Healthcare claim denials are typically categorized into five main types: hard, soft, clinical, technical, and authorization denials. Each category reflects a different cause and determines whether the denial can be corrected or appealed.
- Clinical Denials: These occur when services are deemed not medically necessary or fail coverage criteria. They require strong clinical documentation to appeal.
- Administrative Denials: Common and easier to fix, these denials are caused by errors like incorrect details, missing authorizations, duplicates, or late filing.
- Hard Denials: These refer to determinations where the payer has rejected the claim. Submission of a formal appeal with solid documentation is essential to successfully overturn this denial type and secure payment.
- Soft Denials: These are temporary or conditional denials where payment is withheld pending additional information or corrections; timely resubmission can secure payment.
Reducing claim denials in healthcare starts with understanding how and why they occur.
Common Reasons for Claim Denials and the Solutions
Denied insurance claims commonly occur due to technical issues such as incorrect patient details, missing documentation, or coding errors. Other causes include non-covered services, bundling/unbundling issues, lack of medical necessity, no prior authorization, and missed filing deadlines.
- Eligibility and Coverage Issues
Claims are denied for reasons such as “patient not eligible on the date of service” or “coverage terminated/inactive policy”. This usually occurs when insurance verification is not done correctly before care is provided. It leads to outdated information, changes in coverage, or failure to confirm benefits close to the service date.
Solution: To prevent such denials, providers should verify eligibility upfront, recheck payer portals for real-time updates, and confirm coverage details with the patient. If coverage is inactive, the patient may have to be billed for the service or the claim redirected to an alternative payer, as appropriate.
- Prior Authorization Missing
Prior authorization issues are common for procedures, imaging, and inpatient admissions. They occur when authorization was not obtained in advance or details were entered incorrectly. For example, suppose a patient undergoes an MRI for chronic knee pain, but the provider did not obtain prior authorization from the insurer. The claim is denied with “no prior authorization obtained,” requiring the provider to request retro-authorization or submit clinical documentation to support medical necessity. An “Invalid authorization number” denial occurs if details were not entered correctly.
Solution: To address this, providers can appeal with a request for retro-authorization (if permitted) or submit supporting documentation to demonstrate medical necessity. Retro-authorization or retrospective authorization involves requesting payer approval after a medical service has been performed. It is used in emergencies, administrative delays, or unexpected situations, where prior authorization was not obtained.
- Coding Errors (ICD/CPT Issues)
Coding errors are one of the most frequent causes of claim denials, often stemming from incorrect or mismatched ICD or CPT codes. Common issues include invalid diagnosis codes, procedures that do not align with the documented diagnosis, and upcoding or downcoding discrepancies. These errors not only trigger denials but can also raise compliance concerns if they suggest inaccurate billing practices.
Solution: To address them, providers must ensure strict adherence to medical coding standards, conduct regular audits, and leverage coding validation tools. Correcting the codes and resubmitting claims promptly helps secure reimbursement, while proactive training and technology support reduce the likelihood of repeat denials.
Leveraging AI-powered coding is a proactive way to reduce claim denials by improving both accuracy and speed. It replaces time-consuming manual processes that are prone to errors. For example, the MedGenX AI platform delivers compliant codes in seconds, identifies and corrects coding issues before submission, and captures missed codes to optimize reimbursements. Combined with human-in-the-loop review, it achieves up to 99% accuracy, reduces costly errors and denials, and accelerates the revenue cycle.
- Documentation Problems
Incomplete, unclear, or inconsistent documentation is a major cause of claim denials. Missing details such as provider signatures, insufficient clinical justification, lack of procedure notes, or discrepancies between the diagnosis and services billed can lead payers to reject claims.
Solution: To prevent this, providers should ensure accurate, thorough, and timely documentation that clearly supports medical necessity and aligns with coding and billing requirements.
- Duplicate Claims
Duplicate claim denials occur when a payer flags a submission as already processed. This usually happens when the claim was resubmitted without verifying its current status. “Claim already processed” denials are typically preventable and usually arise due to workflow gaps, such as failing to check claim history or misunderstanding payer remittance codes. While they may seem minor, duplicate denials waste staff time, increase administrative costs, and delay reimbursement.
Solution: The best approach is to verify claim status before resubmission, ensure proper tracking within billing systems, and appeal if a claim was incorrectly marked as a duplicate. Implementing automated claim tracking tools and staff training can further reduce the risk of repeat errors.
- Timely Filing Limits Exceeded
Timely filing denials are a major issue, accounting for 5–10% of all denied claims. Each payer has strict deadlines, ranging from a few months to a year, with variations by insurer, state, and plan type. Missed deadlines cause payment delays, cash flow disruptions, and are often non-recoverable—meaning lost revenue that cannot be appealed or resubmitted.
Solution: When a claim is denied for late filing but was actually submitted on time, providers can appeal by presenting a request to override timely filing based on clear evidence. This includes clearinghouse reports, electronic submission confirmations, payer acknowledgment reports (277CA), or system-generated timestamps showing when the claim was first transmitted. Supporting documents such as claim acceptance logs or batch reports can further strengthen the case. Submitting this proof promptly and in the payer’s required format increases the likelihood of overturning the denial.
- Medical Necessity Denials
Medical necessity denials are among the most complex and challenging for providers. They occur when payers determine that a service, test, or procedure does not meet their coverage criteria or established clinical guidelines. Common reasons include noncompliance with payer policies, insufficient documentation, or lack of evidence supporting medical necessity. These denials often require extensive clinical justification, including detailed physician notes, diagnostic results, and treatment rationale.
Solution: To resolve them, providers must carefully align documentation with payer requirements, ensure coding reflects the clinical scenario accurately, and submit appeals supported by strong medical evidence. Proactive strategies to reduce risk of these denials include educating clinicians on payer policies, using AI-driven documentation support, and conducting pre-authorization checks.
- Bundling / Unbundling Issues
Bundling denials occur when a payer determines that a service is already included in another procedure and should not be billed separately. These are often driven by edits such as the National Correct Coding Initiative (NCCI), which enforces rules to prevent duplicate or overlapping charges.
Solution: Providers must use modifiers correctly to indicate when services are distinct and separately billable. If services were legitimately independent, an appeal with supporting documentation can help overturn the denial. Proactive coding audits and staff training on NCCI edits reduce the risk of repeat errors.
- Coordination of Benefits (COB)
COB denials arise when multiple insurers are involved and the claim was submitted to the wrong payer. For example, a payer may reject a claim if another insurer is considered primary. These denials highlight the importance of verifying insurance coverage and payer hierarchy before submission.
Solution: The corrective action is to determine the correct order of responsibility, rebill to the appropriate insurer, and ensure accurate documentation of coverage. Maintaining up-to-date patient insurance records and using eligibility verification tools can prevent COB-related denials.
- Incorrect Patient Information
Simple administrative errors such as mismatched names, incorrect dates of birth, or invalid subscriber IDs, are common causes of denials. Even small mistakes can have a big impact on cash flow if not addressed promptly. However, while these issues are relatively easy to fix, they take up staff time and delay reimbursement.
Solution: Correcting patient demographics and resubmitting the claim typically resolves the denial. Preventive measures include front-end patient eligibility verification, use of automated data validation tools, and staff training to reduce manual entry errors.
Prevent Denials with Proactive Revenue Cycle Management
Rather than reactive fixes, preventing claim denials is requires a proactive healthcare revenue cycle management strategy. By combining strong front-end processes, accurate coding, real-time eligibility checks, and AI-driven tools, healthcare providers can reduce denials, accelerate reimbursements, and strengthen overall revenue cycle performance.
Reliable denial management services safeguard revenue by turning denial analytics and reporting into proactive strategies that prevent future rejections, accelerate reimbursements, and strengthen overall revenue cycle performance.
Reduce billing errors and optimize your revenue cycle with our denial management services.