Retro Authorization for Emergency vs Non-Emergency Services plays a crucial role in ensuring providers receive proper reimbursement for services already delivered. While prior authorization remains a standard requirement, certain situations require immediate care before approval can be obtained. This is where retro authorization in medical billing becomes essential. Understanding how retrospective approvals work is essential for healthcare providers. Distinguishing between emergency and non-emergency scenarios can help reduce claim denials, maintain compliance, and streamline the revenue cycle.
What Is Retro Authorization in Medical Billing
Retro authorization in medical billing refers to obtaining payer approval after services have already been rendered. Also known as retrospective authorization in healthcare, this process allows providers to demonstrate medical necessity when prior authorization was not obtained due to emergency situations or unavoidable circumstances.
Approval depends on:
- Payer-specific policies
- Documentation quality
- Clinical justification
Without proper documentation, retro authorization requests may be denied.
Emergency vs Non-Emergency Services: Key Differences
Understanding the differences between emergency and non-emergency retro authorization is essential for successful claims management.
Emergency Services
Emergency services involve situations where a patient’s life or health is at immediate risk.
Key Characteristics:
- Prior authorization is typically not required
- Payers allow post-treatment notification
- Retro authorization is more flexible
- Approval depends on documented medical necessity
In most cases, retrospective authorization in healthcare is granted when urgency is clearly documented.
Non-emergency Services
Non-emergency services are planned or elective procedures that require prior approval.
Key Characteristics:
- Prior authorization is mandatory
- Retro authorization is difficult to obtain
- Strict timelines and documentation apply
- Higher risk of claim denial
For non-emergency care, failure to obtain prior authorization is typically considered a provider responsibility.
The differences between emergency and non-emergency retro authorization become evident here.
Common Scenarios Requiring Retro Authorization
Retro authorization is often required when prior approval could not be obtained due to operational or clinical factors.
- Emergency Scenarios
- Unplanned ER visits
- Trauma or accident cases
- Acute conditions (heart attack, stroke, severe infection)
- After-hours admissions
- Emergency transfers
In these cases, retro authorization is generally more lenient when supported by strong documentation.
Non-emergency Scenarios
- Missed prior authorization
- Incorrect insurance information
- System or portal failures
- Delayed eligibility verification
- Changes in treatment plans
- Urgent but non-emergent care
Retro authorization for non-emergency services requires detailed justification and is more likely to face denials.
By understanding these common scenarios, healthcare providers can better prepare for retro authorization requests and improve their chances of claim approval.
Reduce claim denials and streamline your retro authorization process today!
Strengthening Your Retro Authorization Process
Retro Authorization for Emergency vs Non-Emergency Services is a critical component of healthcare billing that bridges patient care and payer compliance.
Emergency cases offer flexibility due to urgency, while non-emergency services require stricter adherence to authorization protocols.
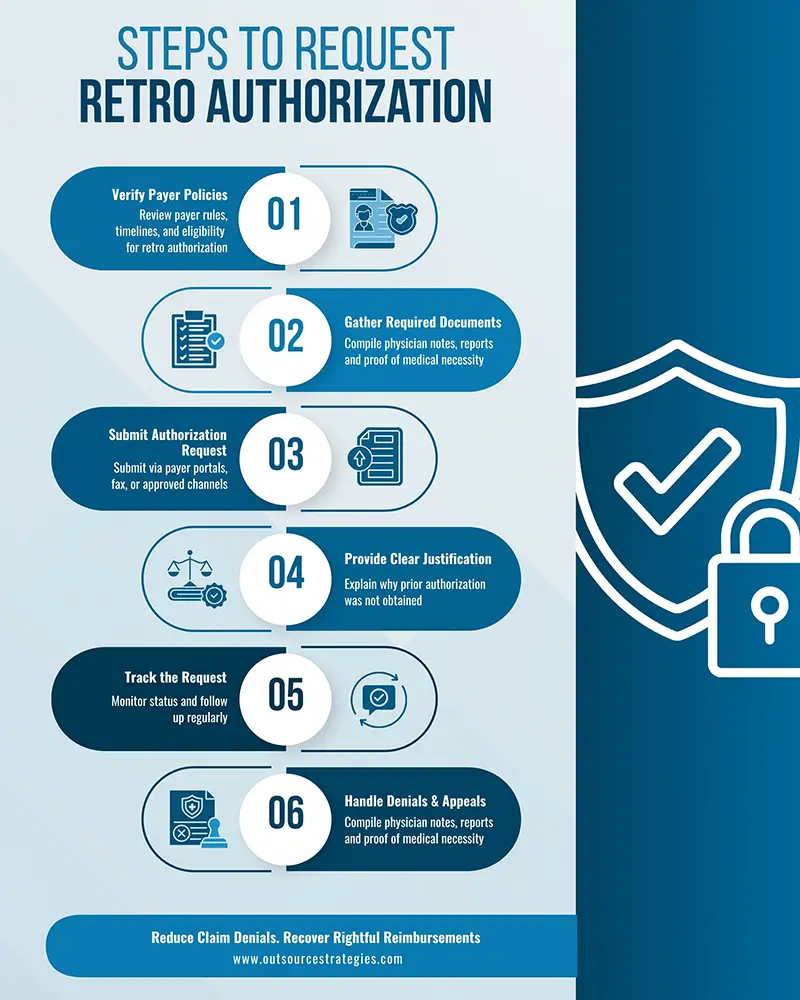
Understanding the differences between emergency and non-emergency retro authorization, along with the steps to request retro authorization in medical billing, helps providers improve reimbursement outcomes and reduce denials.
By optimizing the retro approval process in medical billing, maintaining strong documentation, and adopting efficient workflows, healthcare organizations can navigate retrospective authorization in healthcare more effectively.
Need help managing retro authorization in medical billing?
Contact us to optimize your workflow and improve reimbursement outcomes.